Latest Blogs
Common Eye Diseases and How They Affect Vision
Your eyes are among the most remarkable organs in your body. They help you navigate the world, connect with people, and experience life in full detail. Yet eye health is something many people overlook until a problem becomes hard to ignore. The World Health Organization estimates that over 2.2 billion people worldwide live with some form of vision impairment or blindness. The good news is that a significant proportion of these cases are preventable or treatable when detected early. Understanding common eye diseases, their symptoms, causes, and how they are managed can help you take better care of your vision. What Are Eye Diseases? Eye diseases are medical conditions that affect any part of your eye, including the eyeball, eyelids, eye muscles, and the optic nerve. Some develop quickly and resolve within days. Others are chronic, developing gradually over months or years. Eye diseases are not always limited to the eyes themselves. Many conditions affecting your overall health, such as diabetes and high blood pressure, can directly impact your vision. This is why caring for your general health is also caring for your eyes. Why Eye Health Matters Many eye diseases cause no noticeable symptoms in their early stages. By the time you notice a change in your vision, significant damage may have already occurred. Regular eye examinations allow your eye care specialist to detect conditions before they progress. Early detection can slow or prevent vision loss, preserve your quality of life, and in many cases, allow for simpler treatment options. Common Types of Eye Diseases Refractive Errors Refractive errors are the most common eye conditions worldwide. They occur when the shape of the eye prevents light from focusing correctly on the retina. Types include: Myopia (nearsightedness): You can see nearby objects clearly, but distant objects appear blurry. Hyperopia (farsightedness): Distant objects may appear clearer than close ones. Astigmatism: The cornea or lens has an irregular curve, causing blurred or distorted vision at any distance. Presbyopia: An age-related condition, usually noticed after age 40, where the lens gradually loses its ability to focus on close objects. Refractive errors are typically corrected with prescription glasses, contact lenses, or refractive surgery. Cataracts A cataract is a clouding of the eye's natural lens, which sits behind the iris. It develops slowly, causing vision to become increasingly blurry, cloudy, or dim. Many people describe the experience as looking through a foggy or frosted window. Cataracts are strongly associated with ageing, though other factors such as prolonged UV exposure, smoking, and diabetes can accelerate their development. Surgical removal of the clouded lens and replacement with an artificial one is the standard and highly effective treatment. Learning to recognise cataract symptoms early can make a significant difference in your outcome. Glaucoma Glaucoma is a group of conditions that damage the optic nerve, often due to increased pressure within the eye. It is one of the leading causes of irreversible blindness worldwide. What makes glaucoma particularly concerning is that it typically has no early symptoms. Vision loss often begins at the periphery and gradually closes in, eventually causing tunnel vision if left untreated. Because there are no obvious warning signs in the early stages, regular eye pressure checks and dilated eye exams are the best tools for detection. Age-Related Macular Degeneration (AMD) The macula is the central part of the retina responsible for sharp, detailed vision. AMD damages this area, leading to a gradual loss of central vision. It can make tasks like reading, driving, and recognising faces increasingly difficult. AMD is most common in people over the age of 60 and is influenced by genetics, smoking, and prolonged sun exposure. While there is no cure, certain treatments can slow its progression significantly. Diabetic Retinopathy Diabetic retinopathy is a complication of diabetes that damages the tiny blood vessels in the retina. Over time, these vessels may leak fluid, swell, or grow abnormally, leading to vision distortion and, in severe cases, blindness. People with both Type 1 and Type 2 diabetes are at risk. The condition often shows no symptoms in its early stages, which is why regular eye screenings are recommended for everyone with diabetes. Conjunctivitis Conjunctivitis, commonly known as pink eye, is an inflammation or infection of the conjunctiva, the thin membrane lining the inner surface of the eyelid and the front of the eye. It can be caused by bacteria, viruses, or allergens. Symptoms include redness, itching, discharge, and a gritty feeling in the eye. Some forms of conjunctivitis spread very easily and require prompt treatment to prevent it from passing to others. Eye Infections and Inflammation Beyond conjunctivitis, the eye can be affected by several other infections and inflammatory conditions, including: Blepharitis: Inflammation of the eyelid margins, causing redness, flaking, and irritation. Uveitis: Inflammation of the middle layer of the eye (the uvea), which can develop due to infection or autoimmune conditions. Stye (hordeolum): A painful red lump near the edge of the eyelid caused by a bacterial infection of the oil glands. Keratitis: Inflammation of the cornea, often linked to contact lens misuse or infection. These conditions are usually treatable with medication but should not be ignored, as delayed treatment can lead to complications. Common Symptoms of Eye Diseases Your eyes often communicate changes before you may fully notice them. Watch out for: Blurred, cloudy, or dim vision Sudden changes in vision or sudden vision loss Seeing flashes of light or new floaters (spots or threads drifting across your field of vision) Eye pain, redness, or irritation Double vision Sensitivity to light Halos or rainbow-like rings around lights Difficulty seeing at night Discharge or excessive tearing Some of these symptoms require urgent medical attention. If you experience sudden vision loss, severe eye pain, or a sudden increase in floaters and flashes, seek immediate care. Causes and Risk Factors for Eye Diseases Eye diseases can arise from a wide range of causes: Age: Many eye conditions, including cataracts, AMD, and presbyopia, become more common as you grow older. Genetics: A family history of glaucoma, AMD, or other eye diseases can increase your personal risk. Chronic conditions: Diabetes, high blood pressure, and thyroid disorders are known to affect eye health. UV exposure: Prolonged exposure to ultraviolet light can contribute to cataracts and AMD. Smoking: Nicotine use damages blood vessels throughout the body, including those supplying the eyes. Nutritional deficiencies: Lack of vitamins A, C, E, and minerals like zinc can impair eye health. Eye injuries: Previous trauma to the eye can increase the risk of certain conditions later in life. Ethnicity: Research suggests that certain populations may have a higher predisposition to specific eye conditions. Eye Diseases in Children Children can develop eye conditions that, if not caught early, can affect their development and learning. Some of the most common include: Amblyopia (lazy eye) is a condition where one eye does not develop normal vision, often because the brain favours the stronger eye. It is most effectively treated during early childhood, when the visual system is still developing. Strabismus (squint) refers to a misalignment of the eyes, where both eyes do not look in the same direction simultaneously. Early treatment, which may include glasses, eye patching, or surgery, is important for the best outcomes. Refractive errors are also common in children. A child struggling at school, sitting too close to the board, or squinting frequently may be experiencing uncorrected vision problems. Children may not always realise or express that their vision is unclear. Routine paediatric eye checks are therefore essential, particularly before the school years begin. Eye Diseases in Adults and the Elderly As you age, the risk of developing several significant eye conditions increases. Cataracts and presbyopia are almost universal with age. Glaucoma and AMD become progressively more common after the age of 60. Adults with chronic conditions such as diabetes or hypertension carry an additional risk of eye complications. Managing these underlying conditions, combined with regular eye check-ups, is one of the most effective ways to protect vision in the long term. Even adults with good vision and no apparent symptoms benefit from regular eye examinations, as many conditions remain silent until they have advanced considerably. How Eye Diseases Are Diagnosed Diagnosing an eye disease involves a thorough eye examination and, in some cases, specialised investigations. The typical process includes: Visual acuity test: Assesses how clearly you can see at various distances. Dilated eye exam: Eye drops are used to widen the pupil, allowing the specialist to examine the retina and optic nerve in detail. Slit-lamp examination: A microscope with a bright light gives a magnified view of the structures of the eye. Tonometry: Measures the pressure within the eye, essential for diagnosing glaucoma. Retinal imaging: Detailed photographs of the retina help monitor conditions like diabetic retinopathy and AMD. Optical coherence tomography (OCT): Produces cross-sectional images of the retina, useful for identifying subtle structural changes. Corneal topography: Maps the shape and curvature of the cornea. Blood tests and imaging such as MRI or CT scans may be recommended when an eye condition is linked to a systemic disease. Treatment Options for Eye Diseases Treatment depends on the specific condition and how advanced it is. Options include: Corrective lenses: Glasses or contact lenses correct refractive errors. Prescription eye drops: Used to reduce eye pressure in glaucoma or treat infections. Oral medications: Some inflammatory and infectious eye conditions respond to oral antibiotics or anti-inflammatory drugs. Laser therapy: Used in conditions like glaucoma and diabetic retinopathy to reduce pressure or seal leaking blood vessels. Surgery: Cataract surgery, glaucoma surgery, and vitreoretinal procedures are common surgical interventions for more advanced conditions. Intravitreal injections: Medications injected into the eye, commonly used for AMD and diabetic macular oedema. Vision rehabilitation: For those with irreversible vision loss, support tools and therapy can help maintain independence. Your eye care specialist will recommend the most appropriate treatment based on your diagnosis, age, and overall health. Prevention Tips for Eye Diseases While not all eye diseases can be prevented, you can significantly reduce your risk with a few consistent habits: Schedule regular eye examinations, even if you have no symptoms or do not wear glasses. Wear UV-protective sunglasses when outdoors. Use protective eyewear during sports, construction, or any activity that poses a risk of eye injury. Manage chronic conditions like diabetes and hypertension with proper medical care. Maintain a balanced diet rich in leafy greens, colourful vegetables, oily fish, and foods high in vitamins C and E. Avoid smoking and exposure to tobacco smoke. Practise good hygiene, especially when using contact lenses or touching your eyes. Follow the 20-20-20 rule when working on screens: every 20 minutes, look at something 20 feet away for 20 seconds. This reduces eye strain, though screen time alone is not considered a direct cause of permanent eye disease. Know your family history and share it with your eye care specialist. When to See an Eye Doctor Do not wait for symptoms to worsen before seeking attention. See an eye care professional promptly if you experience: Sudden or rapid vision changes Vision loss in one or both eyes A sudden increase in floaters or flashes of light Severe eye pain or persistent redness Discharge, swelling, or significant sensitivity to light Double vision that appears unexpectedly Even without any of these symptoms, adults should have a routine eye examination at least once every one to two years. If you have diabetes, a family history of glaucoma, or other risk factors, your eye specialist may recommend more frequent checks. Conclusion Your eyes deserve consistent care and attention, not just when something feels wrong. Many serious eye conditions develop silently, making proactive monitoring one of the most important steps you can take for your long-term vision health. Alongside healthy habits, routine health checks can provide valuable insight into your overall wellbeing, including risks that may affect your eyes. At Metropolis Healthcare, you have access to over 4,000 tests, including speciality panels related to diabetes, thyroid health, and other conditions closely linked to eye disease. With home sample collection available across a wide network of touchpoints, easy booking through the website, app, call, or WhatsApp, and accurate reports delivered quickly, staying on top of your health has never been more convenient. Early detection is one of the greatest advantages you can give yourself. Make it a priority. Frequently Asked Questions What Is the Most Common Eye Disease? Refractive errors, including myopia, hyperopia, and astigmatism, are the most common eye conditions worldwide. Cataracts are the leading cause of treatable blindness globally. Both are highly manageable when identified and addressed in time. Can Eye Diseases Be Prevented? Some eye diseases can be prevented or their progression slowed significantly. Wearing UV protection, avoiding smoking, managing chronic conditions like diabetes, eating a nutrient-rich diet, and attending regular eye exams are all effective preventive measures. However, some conditions with a strong genetic component may not be entirely preventable. Are Eye Diseases Hereditary? Yes, several eye diseases have a genetic component. Glaucoma, AMD, and certain types of refractive errors tend to run in families. Knowing your family history allows your eye care specialist to monitor you more closely for specific conditions. Genetic counselling may be recommended in some cases. How Often Should I Get an Eye Exam? Adults with no known eye conditions should have a comprehensive eye exam at least every one to two years. Children should be screened before they start school and at regular intervals thereafter. If you have diabetes, a family history of glaucoma, or other risk factors, your doctor may recommend annual or more frequent check-ups. Can Screen Time Cause Eye Diseases? Prolonged screen use can cause digital eye strain, which leads to symptoms like tired eyes, headaches, and temporary blurred vision. However, current evidence does not support the idea that screen time alone causes permanent eye disease. Practising regular screen breaks, ensuring good lighting, and maintaining an appropriate viewing distance can help reduce strain. If you notice any persistent vision changes, consult an eye care specialist. References World Health Organization. World report on vision. Geneva: WHO; 2019. Flaxman SR, Bourne RRA, Resnikoff S, et al. Global causes of blindness and distance vision impairment 1990-2020: a systematic review and meta-analysis. Lancet Glob Health. 2017;5(12):e1221-e1234. Bourne RRA, Steinmetz JD, Saylan M, et al. Causes of blindness and vision impairment in 2020 and trends over 30 years, and prevalence of avoidable blindness in relation to VISION 2020: the Right to Sight. Lancet Glob Health. 2021;9(2):e144-e160. Tham YC, Li X, Wong TY, Quigley HA, Aung T, Cheng CY. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121(11):2081-2090. Mitchell P, Liew G, Gopinath B, Wong TY. Age-related macular degeneration. Lancet. 2018;392(10153):1147-1159. Yau JW, Rogers SL, Kawasaki R, et al. Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care. 2012;35(3):556-564. Asbell PA, Dualan I, Mindel J, Brocks D, Ahmad M, Epstein S. Age-related cataract. Lancet. 2005;365(9459):599-609.
Hernia Surgery: When It Is Needed and What to Expect
A hernia can feel worrying, especially when it starts affecting your daily life. The good news is that hernia surgery is one of the most commonly performed procedures in the world, with well-established techniques and generally excellent outcomes. Understanding what hernia surgery involves, when it is necessary, and what recovery looks like can help you feel more prepared and less anxious about what lies ahead. What Is Hernia Surgery? A hernia occurs when an internal organ or tissue pushes through a weak spot or opening in the surrounding muscle wall. This often creates a visible or palpable bulge, most commonly in the abdomen or groin area. Hernia surgery, also called herniorrhaphy, is a procedure designed to push the displaced organ or tissue back into its correct position and repair the weakened or torn muscle wall. In many cases, a piece of surgical mesh is used to reinforce the repair and reduce the chance of the hernia returning. Globally, around 20 million hernia surgeries are performed every year, making it one of the most routine surgical procedures in modern medicine. When Is Hernia Surgery Needed? Not every hernia requires immediate surgery. Some hernias are small, cause no discomfort, and may be monitored over time. However, most hernias do worsen gradually, and surgery becomes necessary in the following situations: The hernia causes persistent pain or significant discomfort. The bulge is growing larger over time. The hernia interferes with daily activities, exercise, or work. The hernia cannot be pushed back in (known as an irreducible hernia). There is a risk of strangulation, where blood supply to the trapped tissue is cut off. A strangulated hernia is a medical emergency. If you experience sudden, severe hernia pain, nausea, vomiting, fever, or a rapidly enlarging bulge that turns red or dark, seek emergency care immediately. Recognising hernia symptoms early can help you avoid this serious complication. Even when a hernia is not yet painful, your doctor may recommend surgery to prevent future complications, particularly if the hernia is in a vulnerable location. Types of Hernias That May Need Surgery Several types of hernias may require surgical repair, including: Inguinal hernia: The most common type, occurring in the groin area when tissue pushes through the inguinal canal. It can sometimes extend into the scrotum in men, causing swelling or discomfort. Umbilical hernia: Tissue protrudes near the navel. Common in infants, but also seen in adults. Incisional hernia: Develops through a scar from a previous abdominal surgery. Femoral hernia: Occurs just below the groin, more commonly in women. Hiatal hernia: Part of the stomach pushes up through the diaphragm into the chest cavity. Lumbar and flank hernias: Less common, occurring in the back or side of the abdominal wall. The type of hernia you have influences the surgical approach your doctor will recommend. Types of Hernia Surgery There are three main approaches to hernia repair: Open hernia surgery: The surgeon makes a single incision over the hernia site. The displaced tissue is carefully returned to its proper position, and the abdominal wall defect or weakened muscle is stitched closed, often with surgical mesh for added support. Open surgery is typically used for larger or more complex hernias. Laparoscopic hernia surgery: Also called keyhole surgery, this approach uses three or four small incisions. A thin camera (laparoscope) is inserted through one incision, projecting images onto a monitor. Surgical instruments are passed through the other incisions to complete the repair. This method generally results in less post-operative pain, less scarring, and a faster return to normal activities. Robotic hernia surgery: A form of laparoscopic surgery where the surgeon operates from a console using robotic instruments. It offers greater precision and is particularly useful for complex or recurrent hernias. Robotic repairs may take longer than conventional laparoscopic procedures. Your surgeon will recommend the most appropriate type based on the size, type, and location of your hernia, as well as your overall health. How Hernia Surgery Is Performed Pre-Surgery Preparation Before your surgery, your doctor will conduct a thorough assessment to ensure you are fit for the procedure. Preparation typically involves: A review of your full medical history, including any chronic conditions. A list of all medications, vitamins, and supplements you currently take. Some, particularly blood thinners, may need to be paused before surgery. Blood tests or imaging to assess your overall health. Instructions to fast for a specified period before your procedure. Guidance on stopping smoking if applicable. Smoking increases the risk of infection and can impair healing after surgery. Arranging for someone to drive you home, as you will not be able to drive following anaesthesia. The Surgical Procedure On the day of surgery, you will be given anaesthesia. Open surgery may be performed under local, regional, or general anaesthesia. Laparoscopic and robotic procedures typically require general anaesthesia, meaning you will be asleep throughout. The surgeon will then make the necessary incision or incisions, reposition the herniated tissue, and repair the muscle wall, using sutures, surgical mesh, or both. Once the repair is complete, the incisions are closed and dressed. Simple hernia repairs can take as little as 30 minutes. More complex cases may take several hours. Post-Surgery Monitoring After the procedure, you will be moved to a recovery area where your care team will monitor your vital signs as the anaesthesia wears off. Most hernia surgeries are performed as day procedures, allowing you to go home the same day. More complex repairs may require an overnight hospital stay. Is Surgical Mesh Always Used? Not always, but surgical mesh is used in many hernia repairs. Mesh is a flexible material that reinforces the repaired muscle wall, reducing the likelihood of the hernia returning. It is particularly beneficial for larger hernias or those in areas under significant mechanical stress. In some cases, particularly in young patients or those with small hernias, a surgeon may perform a mesh-free repair using sutures alone. The decision depends on the hernia's characteristics and your individual circumstances. Your surgeon will discuss the approach that best suits your situation. Benefits of Hernia Surgery For those who need it, hernia surgery offers clear advantages: It relieves pain and discomfort caused by the hernia. It prevents the hernia from worsening over time. It eliminates the risk of dangerous complications like strangulation. Minimally invasive techniques mean less scarring and faster recovery for many patients. Research indicates that only around 16% of people require further surgery due to hernia recurrence within 10 years of the first repair. Recovery After Hernia Surgery Recovery varies depending on the type of surgery and the complexity of the repair. In general: You can expect some soreness and discomfort in the first few days after surgery, which is usually manageable with pain relief medication. Light walking is encouraged from the day after surgery to promote circulation and healing. Most people with non-physically demanding jobs can return to work within a few days. Those with physically demanding roles, including jobs that involve lifting, may need to wait several weeks before returning. Driving is typically restricted until you can perform an emergency stop comfortably and are off strong pain medication. Follow-up appointments are important to ensure your wound is healing as expected. How Long Does Recovery Take? Recovery timelines differ from person to person. The size and type of hernia, the surgical method used, your age, and your overall health all play a role. For laparoscopic repairs, many people feel well enough to resume light activities within one to two weeks. Open surgery often involves a longer recovery, sometimes three to six weeks before returning to full activity. Your surgeon will give you a personalised timeline and advise you on when it is safe to resume exercise, heavy lifting, and sexual activity. Always follow their specific guidance rather than general estimates. Risks and Complications of Hernia Surgery Hernia surgery is considered a safe procedure, but as with any operation, it carries some risks. Being informed helps you recognise warning signs early. Short-term risks include: Infection at the incision site. Bruising or bleeding. Fluid collection near the repair site (seroma). Temporary difficulty urinating, particularly after groin hernia repairs. Injury to nearby structures, including blood vessels or the bladder. Longer-term risks include: Chronic pain in the groin or repair area. Mesh-related complications, such as migration or breakdown over time. Hernia recurrence, though this is uncommon. In men who have had inguinal hernia repair, there is a small risk of complications affecting the scrotum or testicular blood flow, though serious outcomes are rare. Anaesthesia-related complications, including cardiovascular events, are rare but can occur. Your surgical team will review your overall health before the procedure to minimise these risks. Activities to Avoid After Hernia Surgery During your recovery, it is important to protect your repair and give your body the time it needs to heal. Avoid the following until your surgeon clears you: Heavy lifting or straining. Vigorous exercise, including running, cycling, or gym training. Driving, particularly in the first few days or while taking strong pain relief. Activities that put direct pressure on the repair site. Sexual activity until advised otherwise. Returning to physically demanding work before you have been assessed. Listen to your body. If something causes pain or discomfort, stop and consult your doctor. When to Call Your Doctor After Surgery Contact your surgeon or healthcare provider if you notice any of the following: Fever or chills. Increasing redness, swelling, or warmth around the wound. Discharge or pus from the incision. Blood seeping through your dressing. Constipation or inability to pass gas that does not resolve. Persistent or worsening pain that is not controlled by prescribed medication. Go to the nearest emergency department immediately if you develop signs of a blood clot in your leg, such as calf pain, sudden swelling, or redness in the leg. Also seek immediate care if you show signs of sepsis, including high fever, rapid heart rate, confusion, or shortness of breath. These are serious conditions requiring urgent attention. Conclusion Hernia surgery is a well-established, effective treatment that can relieve pain, restore normal function, and prevent serious complications. While no surgery is entirely without risk, the procedure has a strong safety record and modern techniques have made recovery faster and more comfortable than ever before. Being well-informed is one of the best things you can do before any medical procedure, and continuing to monitor your overall health is equally important after recovery. At Metropolis Healthcare, preventive health monitoring is made simple and accessible. With over 4,000 tests available, home sample collection across a wide network of touchpoints, and fast, accurate reports, you can stay on top of the health markers that matter most, whether you are preparing for a procedure, recovering from one, or simply looking to understand your health better. Booking is easy through the website, app, call, or WhatsApp. Your health deserves consistent attention. Let Metropolis be your partner in that journey. Frequently Asked Questions Is Hernia Surgery Painful? You will not feel pain during the procedure itself, as anaesthesia is used throughout. After surgery, some soreness and discomfort are expected, particularly in the first few days. This is usually managed effectively with prescribed or over-the-counter pain relief. Laparoscopic surgery typically causes less post-operative pain compared to open surgery. Most people find the discomfort manageable and improve steadily with each passing day. How Long Is the Hospital Stay After Surgery? Most hernia surgeries are performed as day procedures, meaning you go home the same day. More complex repairs, such as those involving large hernias or significant abdominal wall defects, may require an overnight stay of one to two nights. Your surgical team will advise you based on the specifics of your procedure and your recovery in the hours after surgery. Can a Hernia Come Back After Surgery? Yes, hernia recurrence is possible, though it is not common. Research suggests that around 16% of patients may need repeat surgery within 10 years. The use of surgical mesh has significantly reduced recurrence rates. Following your surgeon's post-operative guidance, avoiding heavy lifting during recovery, maintaining a healthy weight, and not smoking all contribute to a better long-term outcome. Is Laparoscopic Hernia Surgery Better Than Open Surgery? Laparoscopic surgery generally offers advantages such as smaller incisions, less post-operative pain, reduced scarring, and a quicker return to normal activities. However, it is not always the most suitable option. Open surgery may be preferable for larger, more complex, or recurrent hernias. The best approach depends on your specific hernia type, size, location, and overall health. Your surgeon will recommend the technique that gives you the best outcome. When Can I Exercise After Hernia Surgery? Light walking can usually begin the day after surgery and is encouraged. However, more strenuous exercise, including weight training, running, and sport, should be avoided until your surgeon gives you the go-ahead. For laparoscopic repairs, this is often around four to six weeks. Open surgery may require a longer wait. Always get personalised guidance from your surgeon before resuming any physical activity. References Fitzgibbons RJ Jr, Giobbie-Hurder A, Gibbs JO, et al. Watchful waiting vs repair of inguinal hernia in minimally symptomatic men: a randomized clinical trial. JAMA. 2006;295(3):285-292. HerniaSurge Group. International guidelines for groin hernia management. Hernia. 2018;22(1):1-165. Bittner R, Schwarz J. Inguinal hernia repair: current surgical techniques. Langenbecks Arch Surg. 2012;397(2):271-282. Kingsnorth A, LeBlanc K. Hernias: inguinal and incisional. Lancet. 2003;362(9395):1561-1571. Amid PK. Lichtenstein tension-free hernioplasty: its inception, evolution, and principles. Hernia. 2004;8(1):1-7. Jenkins JT, O'Dwyer PJ. Inguinal hernias. BMJ. 2008;336(7638):269-272. U.S. Food and Drug Administration. Hernia surgical mesh implants. FDA; 2021.
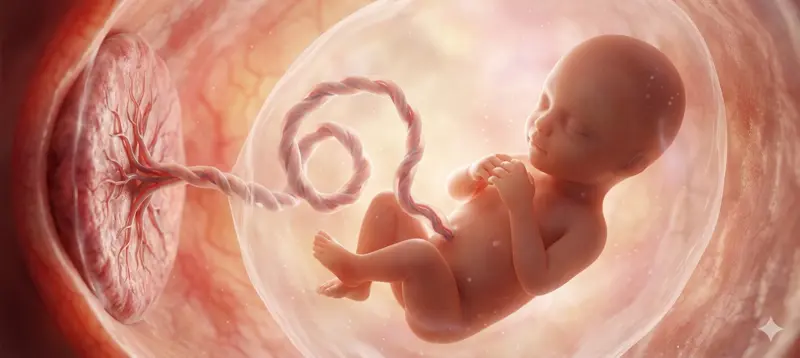
Umbilical Cord: Its Role During Pregnancy
Pregnancy is a remarkable journey, and at the heart of it is a structure that quietly does one of the most important jobs imaginable. The umbilical cord is your baby's lifeline from the very early weeks of pregnancy right up until the moment of birth. Understanding what it does, how it works, and how to care for it after delivery can help you feel more confident and informed throughout this incredible time. What Is the Umbilical Cord? The umbilical cord is a flexible, coiled, rope-like structure that connects your developing baby to the placenta during pregnancy. It is the channel through which everything your baby needs to grow and thrive travels, including oxygen, nutrients, and hormones. At the same time, it carries waste products away from the baby back to the placenta, where your body processes them. After birth, the cord is clamped and cut, leaving a small stump on your baby's tummy. This stump dries up and falls off naturally within a few weeks, and the spot where it was attached becomes your baby's belly button. What Does the Umbilical Cord Do? The umbilical cord performs several essential functions throughout pregnancy: It delivers oxygen-rich blood from the placenta to the fetus, supporting every organ and system as they develop. It provides fetal nutrition, carrying glucose, amino acids, fatty acids, vitamins, and minerals needed for healthy growth. It removes waste products, including carbon dioxide and urea, transporting them from the fetus back to the placenta for your body to eliminate. It transfers antibodies from mother to baby, offering some degree of immune protection. It acts as a flexible, protected channel that accommodates your baby's movements throughout the pregnancy. In essence, the cord acts as the fetus's external circulatory, respiratory, and digestive system all in one, until your baby's own organs are ready to take over at birth. Structure of the Umbilical Cord The umbilical cord is made up of several distinct components: One umbilical vein: This vessel carries oxygenated, nutrient-rich blood from the placenta to the fetus. Two umbilical arteries: These cord blood vessels transport deoxygenated blood and waste products away from the fetus and back to the placenta. Wharton's jelly: A soft, gelatinous connective tissue that surrounds and cushions the three blood vessels, protecting them from compression or twisting caused by fetal movement. Amnion sheath: The outermost covering of the cord, a thin but tough membrane that encases everything within. The cord is naturally coiled along its length, much like a telephone cable. These coils make it stronger and more resistant to kinking or squishing as the baby grows and moves. A typical cord measures between 50 and 60 centimetres in length and around 1 to 2 centimetres in diameter by the end of the second trimester. Where Is the Umbilical Cord Located? The umbilical cord sits within the fluid-filled amniotic sac inside your uterus. One end attaches to the centre of the placenta, the temporary organ anchored to the wall of the uterus. The other end connects to the fetus at what will eventually become the belly button (navel). The placenta itself plays a crucial role in filtering everything that passes through the cord, ensuring that nutrients and oxygen reach the baby while waste products are removed. The cord and placenta work as one integrated system throughout pregnancy. How the Umbilical Cord Supports Fetal Development The cord is far more than a passive tube. It actively supports every stage of fetal development. In the earliest weeks, when the baby's organs are just beginning to form, the cord ensures a steady supply of the nutrients required to build those systems. As the baby grows larger and more complex, the cord keeps pace, expanding to meet increasing demands. Fetal nutrition supplied through the cord fuels not just physical growth but also brain development, bone formation, and the maturation of vital organs such as the heart, lungs, and kidneys. The oxygen delivered through the cord is essential for cell metabolism throughout the body. Because the cord lacks nerves, your baby feels no sensation through it. This means the clamping and cutting of the cord at birth causes no pain whatsoever to your newborn. When Does the Umbilical Cord Form? The umbilical cord begins developing around four weeks into pregnancy, very early in the first trimester. It forms from the same cells that create the placenta and amniotic sac, and it quickly becomes functional as the embryo's needs for nutrients and oxygen grow rapidly in those first weeks. By the end of the first trimester, the cord is well established and continues to grow in length and thickness as the pregnancy progresses. What Happens to the Umbilical Cord After Birth? Immediately after your baby is born, the cord is clamped in two places and then cut between the clamps. This is a routine, painless procedure. It separates your baby from the placenta and marks the moment your newborn begins to breathe, feed, and function independently. A short stump, usually a few centimetres long, is left attached to your baby's navel. Over the following one to three weeks, this stump gradually dries out, shrinks, and changes colour from yellowish-green to brown to black before falling off on its own, revealing the belly button beneath. Delayed Cord Clamping: Benefits and Considerations In recent years, delayed cord clamping has become a topic of growing interest in maternity care. Rather than clamping the cord immediately after birth, some practitioners wait one to three minutes before doing so. During this brief window, blood continues to flow from the placenta into the newborn. Potential benefits of delayed clamping include: Increased iron stores in the newborn, which may reduce the risk of iron deficiency anaemia in the months after birth. Higher levels of stem cells transferred to the baby. Potentially improved outcomes for preterm babies, including better cardiovascular stability. There are situations where immediate clamping remains necessary, such as when the baby or mother requires urgent medical attention. Your obstetric team will advise the approach best suited to your individual circumstances. Umbilical Cord Care After Birth Once you are home with your newborn, caring for the cord stump properly helps prevent infection and supports natural healing. Give your baby sponge baths only until the stump falls off. Avoid submerging the stump in water. Keep the stump clean and dry. Allow it to air dry after cleaning. Fold the front of the nappy down and away from the stump to prevent contact with urine or stool. If the stump gets soiled, wipe it gently with a damp cloth and allow it to dry completely. Let the stump fall off naturally. Do not attempt to pull it off, even if it appears to be hanging by a thread. Avoid applying alcohol to the stump. Current guidance advises against this, as it may interfere with the natural separation process. Dress your baby in loose clothing that does not rub against the stump. Signs of Infection in the Umbilical Stump The stump will change in appearance as it heals, but certain signs suggest infection and require prompt medical attention. Contact your paediatrician if you notice: Increasing redness or discolouration of the skin around the stump. Swelling at or near the base of the stump. Pus, cloudy fluid, or a foul smell coming from the stump. Bleeding that does not stop when gently wiped. Your baby has a fever or appears unusually unwell. Your baby cries when the stump or surrounding skin is touched. The stump has not fallen off after three weeks. Common Umbilical Cord Problems During Pregnancy Most pregnancies involve a cord that functions without any difficulty. However, certain conditions can arise that may affect blood flow or delivery: Nuchal cord: The cord loops around the fetus's neck. A loose loop is usually harmless, but a tight one can occasionally cause complications during labour. True knot: A genuine knot forms in the cord. Tight knots can restrict blood flow to the baby. Cord prolapse: The cord slips into the birth canal ahead of the baby, which can compress it during contractions. This is a medical emergency requiring immediate delivery, usually by caesarean section. Single umbilical artery: The cord contains only one artery instead of two. This can be associated with certain genetic conditions or structural changes in the baby's organs and warrants close monitoring. Abnormal cord coiling: Too many or too few coils in the cord, which may be linked to changes in fetal movement or blood flow. Umbilical cord cysts: Fluid-filled sacs within the cord. These are often harmless but may occasionally press on the vessels. Velamentous cord insertion: The cord attaches to the membranes outside the placenta rather than to the placenta itself, which can affect fetal growth. Vasa praevia: Unprotected cord vessels cross the cervical opening. This is a serious condition that requires early diagnosis and planned caesarean delivery. Many of these complications are rare. Your prenatal team monitors your pregnancy closely and uses ultrasound to identify any concerns early. How Umbilical Cord Problems Are Diagnosed Ultrasound Examination Routine ultrasound scans during pregnancy allow your doctor to examine the umbilical cord's attachment to the placenta, the number of vessels present, and the general appearance of the cord. Many cord abnormalities are identified during these standard scans, sometimes before any symptoms arise. Doppler Studies Doppler ultrasound measures blood flow through the umbilical vessels. It is particularly useful when fetal growth restriction is a concern, as reduced or abnormal blood flow through the cord can be an early indicator that the baby is not receiving adequate nourishment. Doppler studies are a non-invasive and safe way to assess how well the cord is functioning. Monitoring During Labour During labour, your baby's heart rate is continuously monitored using a cardiotocograph (CTG). Changes in the heart rate pattern can suggest cord compression or reduced blood flow and allow the team to respond quickly if intervention is needed. Umbilical Cord Blood Banking Cord blood is the blood remaining in the umbilical cord and placenta after birth. It is rich in stem cells, which have the potential to develop into various types of blood cells and may be used in the treatment of certain medical conditions. Parents have the option of donating cord blood to a public bank, where it may be used by patients in need, or storing it privately for potential future use by their family. Benefits of Cord Blood Storage Cord blood stem cells can be used in the treatment of certain blood disorders, immune conditions, and some cancers. It is a non-invasive collection process that poses no risk to the mother or baby. Privately stored cord blood offers a potentially compatible stem cell match for the child or certain family members. It is collected at the time of birth and cannot be retrieved later, making the decision a time-sensitive one. It is worth discussing cord blood banking with your obstetrician during pregnancy so you can make an informed decision in advance of your due date. Pregnancy Care Tips While many cord-related conditions are not preventable, certain habits during pregnancy support overall fetal wellbeing and reduce avoidable risks: Attend all scheduled prenatal appointments and ultrasound scans. Report any significant reduction in your baby's movements to your midwife or doctor promptly. Maintain a nutritious, balanced diet to support healthy placental function and fetal growth. Avoid smoking, alcohol, and recreational substances, all of which can impair blood flow and fetal development. Manage any pre-existing conditions such as diabetes or hypertension with the guidance of your healthcare team, as these can affect placental and cord health. Sleep on your side during the later stages of pregnancy, as this supports optimal blood flow to the baby. Seek immediate care if you experience unusual pain, bleeding, or a sudden change in fetal movement. When to Consult a Doctor During pregnancy, contact your doctor or midwife if you notice: A significant or sudden decrease in your baby's movements. Unusual abdominal pain or cramping. Vaginal bleeding at any stage. Leaking fluid before your due date. After birth, contact your paediatrician if the cord stump shows signs of infection, bleeds persistently, or has not fallen off within three weeks of birth. Any concerns, however small, are always worth raising with your healthcare provider. Trust your instincts as a parent. Conclusion The umbilical cord is one of nature's most elegant solutions, a small but extraordinary structure that sustains your baby's life from the earliest weeks of pregnancy until the very moment of birth. Understanding its role, recognising potential concerns, and knowing how to care for the cord stump after delivery are all part of being well-prepared for your journey into parenthood. Staying healthy throughout pregnancy also means staying informed about the markers that shape your overall wellbeing. At Metropolis Healthcare, you can access a wide range of speciality tests and health screenings, including those relevant to pregnancy and maternal health, all from the comfort of your home through a trusted home sample collection network. With over 4,000 tests, fast and accurate reports, and easy booking available through the website, app, call, or WhatsApp, Metropolis makes proactive health monitoring simple at every stage of life. A healthy pregnancy begins with consistent care, for both you and your baby. Frequently Asked Questions What Is the Main Function of the Umbilical Cord? The umbilical cord's primary function is to connect the developing fetus to the placenta, enabling the transfer of oxygen and nutrients from the mother to the baby, and carrying waste products such as carbon dioxide away from the fetus. It is the essential channel through which all fetal nourishment travels throughout pregnancy. Does Cutting the Cord Hurt the Baby? No. The umbilical cord does not contain any nerves, which means your baby has no sensation in the cord at all. Clamping and cutting the cord at birth is completely painless for your newborn. Similarly, as the stump dries and falls off in the weeks after birth, your baby will not feel any discomfort from the process. Can Umbilical Cord Issues Affect Baby Health? Yes, in some cases. Conditions such as cord prolapse, true knots, or vasa praevia can restrict blood flow to the baby or create complications during delivery. A single umbilical artery may be associated with certain chromosomal or structural conditions. However, many cord variations are harmless, and regular prenatal monitoring means most problems are identified and managed early. How Long Does the Stump Take to Fall Off? The umbilical cord stump typically dries up and falls off within one to three weeks of birth. During this time, it will change colour from yellowish-green to brown to black as it shrinks. If the stump has not separated by three weeks, or if you notice signs of infection, it is important to consult your paediatrician. Can Babies Survive Cord Complications? Many cord complications, when identified and managed early, do not lead to lasting harm. Conditions like a loose nuchal cord or minor cord cysts are usually monitored without intervention. More serious complications such as cord prolapse or vasa praevia require immediate medical attention but are manageable with prompt action. Early diagnosis through regular prenatal care is the most important factor in ensuring good outcomes. Is Cord Blood Banking Necessary? Cord blood banking is not a medical requirement, but it is a personal decision some families make. Cord blood contains stem cells that may be valuable in treating certain conditions in the future. Public donation means the blood can help any patient in need, while private banking preserves it specifically for your family. Discussing the options with your doctor before your due date will help you decide what is right for your circumstances. References Benirschke K, Burton GJ, Baergen RN. Pathology of the Human Placenta. 6th ed. Springer; 2012. Umbilical cord abnormalities. StatPearls. National Library of Medicine; 2023. Delayed umbilical cord clamping after birth. Committee Opinion No. 814. Obstet Gynecol. 2020;136(6):e100-e106. Pappa KI, Anagnou NP. Novel sources of fetal stem cells: where do they fit on the developmental continuum? Regen Med. 2009;4(3):423-433. World Health Organization. WHO recommendations for care of the preterm or low-birth-weight infant. Geneva: WHO; 2022. Hasegawa J, Matsuoka R, Ichizuka K, et al. Umbilical cord complications during labor. J Obstet Gynaecol Res. 2009;35(5):826-829. McDonald SJ, Middleton P, Dowswell T, Morris PS. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev. 2013;7:CD004074.
Endometrial Thickness: What Is Normal and What Is Not
Your body goes through extraordinary changes every month, and the lining of your uterus is at the centre of much of that activity. Endometrial thickness is a term you may have encountered during an ultrasound, a fertility consultation, or a routine gynaecological check-up. Understanding what it means, what is considered normal at different stages of life, and when to seek advice can help you stay informed and in control of your reproductive health. What Is Endometrial Thickness? Endometrial thickness refers to the measured depth of the endometrium, the tissue lining the inner wall of the uterus. This measurement is taken using ultrasound and reflects how thick or thin the lining is at any given point in time. The endometrium is not a static structure. It grows, thickens, and sheds in response to hormonal signals throughout the menstrual cycle. Its thickness is therefore a dynamic value that changes depending on where you are in your cycle, your age, your hormonal status, and whether you are pregnant or post-menopausal. Measuring endometrial thickness is a key diagnostic tool. It helps doctors assess reproductive health, investigate abnormal uterine bleeding, evaluate fertility, and screen for conditions such as endometrial hyperplasia or endometrial cancer. What Is the Endometrium? The endometrium is the innermost lining of the uterus. It is a highly specialised tissue that responds to the hormones oestrogen and progesterone throughout each menstrual cycle. Each month, the endometrium thickens in preparation for a potential pregnancy. If a fertilised egg does not implant, progesterone levels fall, and the lining sheds as menstrual bleeding. If implantation does occur, the endometrium plays a critical role in nourishing the developing embryo in the early weeks of pregnancy, before the placenta fully takes over. The endometrium has two main layers. The functional layer is the outer layer that grows, thickens, and sheds each cycle. The basal layer beneath it remains relatively stable and gives rise to the functional layer each new cycle. How Endometrial Thickness Changes During the Menstrual Cycle The menstrual cycle lining undergoes predictable changes driven by hormonal fluctuations. Understanding these changes helps contextualise what thickness readings mean: Menstrual phase (Days 1 to 5): The functional layer sheds, and the endometrium is at its thinnest, typically between 2 and 4 mm. Early proliferative phase (Days 6 to 9): Oestrogen begins to rise, stimulating the endometrium to rebuild. Thickness increases to around 5 to 7 mm. Late proliferative phase (Days 10 to 14): As ovulation approaches, oestrogen peaks and the endometrium continues to thicken, reaching approximately 8 to 11 mm. It takes on a characteristic layered appearance on ultrasound. Secretory phase (Days 15 to 28): After ovulation, progesterone takes over. The endometrium thickens further and becomes more uniform, reaching up to 16 mm. It is during this phase that the lining is at its most receptive for implantation. Normal Endometrial Thickness Range Normal Thickness in Women of Reproductive Age In women who are menstruating regularly, endometrial thickness is considered normal when it falls within the expected range for the corresponding phase of the cycle. During any phase of the cycle, a thickness below 14 mm is generally considered within normal limits. The thinnest acceptable measurement during the menstrual phase is around 2 mm. At the height of the secretory phase, up to 16 mm is within the normal range. These figures provide a broad window, and your doctor will always interpret your reading in the context of where you are in your cycle and any symptoms you may have. Normal Thickness After Menopause After menopause, the endometrium no longer cycles through monthly changes. Without the stimulation of oestrogen produced by active ovaries, the lining becomes thin and atrophic. A normal endometrial thickness for postmenopausal women not taking hormone replacement therapy (HRT) is 5 mm or less. For postmenopausal women on HRT, the lining may measure slightly thicker, sometimes up to 8 mm, depending on the type and duration of therapy. Any reading above 5 mm in a postmenopausal woman who is not on HRT, particularly when accompanied by bleeding, warrants further investigation. Endometrial Thickness in Pregnancy During early pregnancy, the endometrium does not shed. Instead, it continues to thicken to support the developing embryo. For women undergoing fertility treatment, an endometrial thickness of 8 to 15 mm is generally considered the ideal range for embryo implantation. A very thin endometrium, typically below 7 mm, is associated with lower implantation rates, a higher risk of early miscarriage, and potential placental complications. A lining that is excessively thick may also affect implantation outcomes. Your fertility specialist will assess your specific measurements in the context of your overall treatment plan. How Endometrial Thickness Is Measured The standard method for measuring endometrial thickness is ultrasound, which is safe, non-invasive, and widely available. The process typically involves: Transvaginal ultrasound: A small, smooth probe is gently inserted into the vagina. This method provides the most accurate and detailed view of the uterine lining and is preferred in most clinical settings. Transabdominal ultrasound: The probe is placed on the lower abdomen. This is less precise for endometrial measurements but may be used when a transvaginal scan is not appropriate. MRI: Magnetic resonance imaging is used when ultrasound is not suitable, for example due to the position of the uterus or the presence of fibroids that obscure the view. MRI provides detailed images of uterine structures. Hysteroscopy: A thin telescope is passed into the uterus through the cervix, allowing direct visualisation of the endometrium. It is typically used when a tissue biopsy is also needed. Endometrial biopsy: A small sample of endometrial tissue is taken for laboratory analysis. This is used when abnormal thickening or bleeding requires histological assessment to rule out hyperplasia or cancer. Endometrial Thickness and Fertility The thickness and quality of the endometrium are important factors in achieving a successful pregnancy. For natural conception and assisted reproductive techniques alike, the uterine lining must be sufficiently thick, well-vascularised, and receptive to allow an embryo to implant and develop. Ideal Endometrial Thickness for Pregnancy For women undergoing IVF or frozen embryo transfer, most fertility specialists consider a thickness of 7 to 10 mm optimal at the time of transfer. Some studies suggest that a minimum of 6 to 7 mm is associated with reasonable implantation rates, while a lining below 6 mm is associated with significantly poorer outcomes. It is important to note that thickness alone is not the only measure of endometrial receptivity. Blood flow to the lining, the pattern seen on ultrasound, and hormonal levels are all considered together when assessing readiness for implantation. Causes of a Thick Endometrium A thicker than expected endometrium can have several underlying causes: Elevated oestrogen levels without adequate progesterone to counterbalance them. Endometrial hyperplasia, a condition where the lining overgrows and can, in some cases, progress to cancer. Endometrial polyps, which are localised overgrowths of the endometrial lining. Endometrial cancer, which is one of the more serious causes of significant thickening. Obesity, which leads to higher circulating oestrogen levels from fatty tissue. Diabetes and high blood pressure, both of which are associated with increased endometrial thickness. Tamoxifen use, a medication used in breast cancer treatment that has oestrogen-like effects on the uterus. Hormone replacement therapy, particularly unopposed oestrogen therapy. Early pregnancy or ectopic pregnancy. Causes of a Thin Endometrium A thinner than expected endometrium can also be caused by several factors: Low oestrogen levels, which may occur as a result of premature ovarian insufficiency or surgical menopause. Ageing and natural menopause. Previous uterine procedures or infections that have caused scarring, a condition known as Asherman's syndrome. Prolonged use of certain medications, including some contraceptives. Poor blood flow to the uterus. Chronic inflammation of the uterine lining (chronic endometritis). A thin endometrium is associated with difficulty conceiving and a higher risk of miscarriage when pregnancy does occur. Symptoms Associated with Abnormal Thickness The endometrium does not always give obvious signals when something is wrong. However, the following symptoms may suggest that your endometrial thickness is outside the normal range and warrant medical assessment: Abnormal uterine bleeding, including unusually heavy or prolonged periods. Spotting or bleeding between periods. Vaginal bleeding or spotting after menopause. Irregular menstrual cycles that are shorter than 21 days or longer than 38 days. Absence of periods (amenorrhoea) in women of reproductive age. Pelvic pain or a sense of pressure in the lower abdomen. A feeling of fullness or bloating without an obvious dietary cause. Any of these symptoms should prompt a visit to your gynaecologist for evaluation. Endometrial Thickness vs Endometrial Hyperplasia Feature Normal Endometrial Thickness Endometrial Hyperplasia Definition Natural variation in lining depth across the cycle Abnormal overgrowth of the endometrial lining Cause Hormonal cycling (oestrogen and progesterone) Excess oestrogen, often without progesterone opposition Thickness range 2 to 16 mm depending on cycle phase Often above 16 mm; may vary Cancer risk None Possible, particularly with atypical hyperplasia Symptoms None; normal monthly variation Irregular bleeding, heavy periods, postmenopausal bleeding Management Monitoring and routine care Medical or surgical treatment depending on severity Endometrial Thickness vs Uterine Fibroids Feature Abnormal Endometrial Thickness Uterine Fibroids Location Endometrial lining (inner uterus) Uterine muscle wall (myometrium) Nature Thickening of existing tissue Separate benign growths of muscular tissue Effect on lining Directly involves the endometrium May distort the uterine cavity or compress the lining Symptoms Abnormal bleeding, pelvic pain Heavy bleeding, pelvic pressure, bladder symptoms Diagnosis Ultrasound, endometrial biopsy Ultrasound, MRI Fertility impact Can impair implantation May affect implantation depending on location and size Treatment for Abnormal Endometrial Thickness Treatment depends on whether the endometrium is too thick or too thin, and what is causing the abnormality. For a thick endometrium: Progestin therapy to counterbalance oestrogen and reduce the thickness. Hormonal contraceptives to regulate the cycle and control endometrial growth. Removal of polyps or fibroids via hysteroscopy if these are contributing to thickening. In cases of hyperplasia or cancer, more definitive treatment including surgery (hysterectomy) may be recommended. Lifestyle changes such as achieving a healthier body weight, which can reduce excess oestrogen levels. For a thin endometrium: Oestrogen therapy to stimulate endometrial growth. Medications or supplements to improve blood flow to the uterine lining. Treatment of underlying conditions such as chronic endometritis with antibiotics. In fertility treatment, adjustments to stimulation protocols to optimise lining thickness before embryo transfer. It is important to note that treatments for thin endometrium do not always produce consistent results. Your specialist will work with you to find the most appropriate approach based on your individual situation. Endometrial Thickness After Menopause After menopause, the gradual decline in oestrogen causes the endometrium to become thin and inactive. A lining of 5 mm or less is considered normal for postmenopausal women who are not on HRT. Any bleeding after menopause is not normal and should be investigated promptly, regardless of what the endometrial thickness measures. While a thin lining is reassuring, postmenopausal bleeding is a symptom that always requires evaluation to rule out endometrial cancer. Women on HRT may have a slightly thicker lining, as oestrogen continues to stimulate the endometrium. The type of HRT matters. Combined oestrogen and progesterone therapy is generally considered safer for the endometrium than oestrogen-only therapy in women who still have a uterus. When to Worry About Endometrial Thickness Not all variations in endometrial thickness are cause for concern. However, there are situations where further investigation is important: A thickness above 5 mm in a postmenopausal woman not on HRT. Any postmenopausal bleeding, regardless of the thickness reading. A thickness persistently outside the expected range for your cycle phase. Abnormal uterine bleeding in a woman of reproductive age that is not explained by normal hormonal cycling. A reading above 16 mm outside of the secretory phase. An unusually thin lining during fertility treatment that is not responding to therapy. When to See a Gynaecologist Do not delay seeking medical advice if you notice any of the following: Bleeding after menopause, even if it appears light or brief. Periods that are significantly heavier or longer than usual. Spotting between periods that is new or persistent. Pelvic pain that is unexplained or worsening. Difficulty conceiving after several months of trying. A previous scan showing an abnormal endometrial thickness that has not been followed up. Any symptoms that feel unusual for you, even if they do not appear on this list. Your gynaecologist can arrange the appropriate investigations and interpret your results in the full context of your health history. Conclusion Endometrial thickness is a meaningful window into your reproductive and hormonal health. Whether you are in your fertile years, trying to conceive, approaching menopause, or beyond it, keeping track of changes and seeking prompt advice when something seems different is always the right approach. Awareness is only part of the picture. Regular health monitoring allows you to stay ahead of changes before they become bigger concerns. At Metropolis Healthcare, a wide range of speciality tests are available to support women's health at every stage of life, from hormonal panels to comprehensive full body checkups. With home sample collection across an extensive network, fast and accurate reports, and easy booking through the website, app, call, or WhatsApp, taking care of your health has never been more straightforward. Your health deserves consistent attention. Start with knowing your numbers. Frequently Asked Questions What Is Normal Endometrial Thickness? Normal endometrial thickness varies depending on where you are in your menstrual cycle or life stage. During menstruation, 2 to 4 mm is typical. In the proliferative phase, it rises to around 5 to 11 mm, and in the secretory phase, up to 16 mm is considered normal. For postmenopausal women not on HRT, 5 mm or less is the accepted normal range. Can Endometrial Thickness Be Improved Naturally? Some lifestyle factors may support endometrial health. Maintaining a healthy weight helps regulate oestrogen levels. A nutrient-rich diet that includes iron, healthy fats, and antioxidants supports hormonal balance. Regular moderate exercise and avoiding smoking may also contribute to better uterine blood flow. However, these measures are supportive and not a substitute for medical treatment when a clinical abnormality is identified. Is a Thick Endometrium Cancerous? Not necessarily. A thick endometrium can result from many causes, including normal hormonal fluctuation, the use of certain medications, obesity, or benign conditions like polyps. However, a significantly thickened lining, particularly in postmenopausal women or those with abnormal bleeding, does require investigation. Endometrial hyperplasia and endometrial cancer are among the conditions that can present with an abnormally thick lining, which is why evaluation by a doctor is important. Can a Thin Endometrium Cause Infertility? Yes, it can. A thin endometrium, typically defined as below 7 mm, is associated with reduced implantation rates, higher rates of early pregnancy loss, and in some cases, difficulty achieving conception at all. A well-prepared endometrium is essential for a fertilised egg to implant and develop successfully. Women undergoing fertility treatment will have their lining assessed carefully before embryo transfer. How Can I Increase Endometrial Thickness Naturally? Some approaches may help support endometrial growth. Oestrogen-supporting foods such as flaxseeds, soy, and certain leafy vegetables may play a role. Improving blood flow through regular exercise, adequate hydration, and avoiding smoking can also be beneficial. Acupuncture is sometimes explored by women undergoing fertility treatment, though evidence is still emerging. Medical options such as oestrogen therapy are available for women with clinically thin endometrium and should be discussed with a specialist. Does Endometrial Thickness Vary Monthly? Yes, it does. Endometrial thickness changes predictably throughout the menstrual cycle in response to oestrogen and progesterone. It is at its thinnest during menstruation and at its thickest in the secretory phase before the next period begins. This monthly variation is entirely normal and is what makes the endometrium a dynamic, responsive tissue rather than a fixed measurement. References Munro MG, Critchley HOD, Fraser IS; FIGO Menstrual Disorders Committee. The two FIGO systems for normal and abnormal uterine bleeding symptoms and classification of causes of abnormal uterine bleeding in the reproductive years. Int J Gynaecol Obstet. 2018;143(3):393-408. Nalaboff KM, Pellerito JS, Ben-Levi E. Imaging the endometrium: disease and normal variants. Radiographics. 2001;21(6):1409-1424. Leone FPG, Timmerman D, Bourne T, et al. Terms, definitions and measurements to describe the sonographic features of the endometrium and intrauterine lesions. Ultrasound Obstet Gynecol. 2010;35(1):103-112. Goldstein SR. The role of transvaginal ultrasound or endometrial biopsy in the evaluation of the menopausal endometrium. Am J Obstet Gynecol. 2009;201(1):5-11. Kasius A, Smit JG, Torrance HL, et al. Endometrial thickness and pregnancy rates after IVF: a systematic review and meta-analysis. Hum Reprod Update. 2014;20(4):530-541. Kurman RJ, Kaminski PF, Norris HJ. The behavior of endometrial hyperplasia: a long-term study of untreated hyperplasia in 170 patients. Cancer. 1985;56(2):403-412. American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 149: Endometrial cancer. Obstet Gynecol. 2015;125(4):1006-1026.
Hypoxia: What Happens When the Body Lacks Oxygen
Breathing is something most of us do without a second thought. Yet every breath you take sets off a precise chain of events that keeps every cell, tissue, and organ in your body alive. When that chain is disrupted and oxygen levels fall too low, the result is a condition called hypoxia. It can develop gradually or strike suddenly, and without prompt attention, it can become life-threatening. Understanding what hypoxia is, what causes it, and what to do about it could make a critical difference for you or someone you care about. What Is Hypoxia? Hypoxia is a condition in which the body's tissues and organs do not receive enough oxygen to function properly. It is not simply about difficulty breathing. Even if you are breathing normally, hypoxia can occur if oxygen is not being absorbed into the blood effectively, if the blood cannot carry it adequately, or if the tissues cannot use it as they should. Every organ in your body depends on a continuous supply of oxygen to produce energy, repair cells, and carry out its functions. When that supply falls short, the consequences can range from mild discomfort to severe organ damage, depending on how long the oxygen deprivation lasts and which tissues are affected. Hypoxia is different from hypoxemia, though the two are closely related. Hypoxemia refers specifically to low oxygen levels in the blood, while hypoxia refers to insufficient oxygen at the tissue level. Hypoxemia is one of the most common causes of hypoxia. What Happens When Oxygen Levels Drop? When oxygen delivery to the tissues is compromised, your body responds quickly. Your heart rate increases to pump more blood. Your breathing speeds up to try to draw in more oxygen. Your body may redirect blood flow away from non-essential areas towards vital organs like the brain and heart. If these compensatory mechanisms are not enough, cells begin to fail. Without oxygen, cells cannot produce the energy they need to sustain their functions. Within minutes, particularly in oxygen-sensitive tissues like the brain, cell damage begins. Brain cells can start to die within five minutes of severe oxygen deprivation. The heart, kidneys, and liver are also highly vulnerable. This is why hypoxia is never something to wait out or observe at home without medical guidance. The faster it is recognised and treated, the better the chances of a full recovery. Types of Hypoxia Hypoxia is not a single, uniform condition. It can arise through four distinct mechanisms: Hypoxaemic hypoxia: The most common type, caused by low levels of oxygen in the blood. This occurs when the lungs cannot transfer enough oxygen into the bloodstream, often due to conditions such as pneumonia, asthma, or chronic obstructive pulmonary disease (COPD). Travelling to high altitudes, where the air contains less oxygen, can also cause this type. Circulatory (ischaemic) hypoxia: The blood may carry adequate oxygen, but a problem with the heart or blood vessels prevents it from reaching the tissues in sufficient quantities. Heart failure, blood clots, and severe narrowing of blood vessels are common causes. Anaemic hypoxia: The body does not have enough healthy red blood cells to carry oxygen from the lungs to other tissues. This can occur in various forms of anaemia, where red blood cells are too few, misshapen, or ineffective. Histotoxic hypoxia: Oxygen reaches the tissues in normal amounts, but the cells are unable to use it properly. Cyanide poisoning is a classic example of this type, where cellular machinery for oxygen use is disrupted. Common Causes of Hypoxia Any condition that affects oxygen intake, transport, or use at the cellular level can lead to hypoxia. Common causes include: Asthma, particularly during a severe attack. COPD and emphysema. Pneumonia and other serious lung infections. Pulmonary embolism, a blood clot in the lung that obstructs blood flow. Pulmonary oedema, where fluid accumulates in the lungs. Pulmonary fibrosis, a condition involving progressive scarring of lung tissue. Congestive heart failure, where the heart cannot pump blood efficiently. Congenital heart disease, particularly when there is abnormal mixing of oxygenated and deoxygenated blood. Sleep apnoea, which causes repeated drops in oxygen during sleep. Severe anaemia. Exposure to high altitudes. Certain medications that suppress breathing. COVID-19 and influenza, which can cause significant respiratory complications. Symptoms of Hypoxia Symptoms vary depending on how severe the oxygen deprivation is and how quickly it develops. In mild or chronic hypoxia, symptoms may be subtle and easy to overlook. In acute or severe cases, they can escalate rapidly. Common symptoms include: Shortness of breath or difficulty breathing, even at rest. Rapid breathing (more than 20 breaths per minute). Rapid heart rate (tachycardia). Restlessness or a sense of agitation. Headache. Confusion or difficulty concentrating. Anxiety without an obvious cause. Fatigue and weakness. Bluish or greyish discolouration of the lips, fingernails, or skin, a sign called cyanosis. In severe hypoxia, you may notice an abnormally slow heart rate, extreme restlessness, or loss of consciousness. These are signs of a medical emergency requiring immediate care. Hypoxia in Newborns Newborns are particularly vulnerable to hypoxia. Perinatal hypoxia, where a baby does not receive adequate oxygen around the time of birth, can occur due to complications during labour and delivery, such as umbilical cord problems, placental issues, or prolonged difficult delivery. The consequences in newborns can be serious. The brain is especially sensitive, and oxygen deprivation at this stage can affect neurological development, sometimes resulting in conditions such as hypoxic-ischaemic encephalopathy (HIE). Medical teams are trained to monitor oxygen levels closely during and after delivery and to act swiftly if signs of distress appear. If you are pregnant and have concerns about your baby's movements or wellbeing at any stage, do not hesitate to contact your midwife or obstetrician. Early intervention matters enormously. Hypoxia at High Altitude Travelling to or living at high altitudes exposes the body to air that contains lower concentrations of oxygen. This can lead to a form of hypoxaemia and result in altitude sickness, characterised by headache, nausea, fatigue, dizziness, and shortness of breath. In most healthy individuals, symptoms are mild and improve as the body acclimatises over a few days. However, in more serious cases, high-altitude pulmonary oedema (HAPE) or high-altitude cerebral oedema (HACE) can develop, both of which are medical emergencies. If you have a pre-existing heart or lung condition, speak to your doctor before travelling to high-altitude destinations. Gradual ascent, adequate hydration, and avoiding strenuous activity in the first few days can all reduce the risk of altitude-related hypoxia in otherwise healthy travellers. How Hypoxia Is Diagnosed When hypoxia is suspected, your doctor will carry out a physical examination and may recommend a series of investigations to confirm the diagnosis and identify its underlying cause. Physical examination: Your doctor will listen to your heart and lungs, assess your breathing pattern, and check your skin, lips, and nails for signs of cyanosis or poor circulation. Pulse oximetry: A small, painless clip placed on your fingertip measures the percentage of oxygen in your blood. A normal reading is typically 95% or above. Readings below 90% are considered concerning. Arterial blood gas (ABG) test: A blood sample taken from an artery provides precise measurements of oxygen and carbon dioxide levels, as well as blood pH, giving a detailed picture of respiratory and metabolic status. Pulmonary function tests (PFTs): These measure how well your lungs are working, including how much air you can breathe in and out and how efficiently oxygen crosses into the bloodstream. Imaging: Chest X-rays, CT scans, or ventilation-perfusion (VQ) scans help visualise the lungs and identify conditions such as pneumonia, fluid, clots, or structural abnormalities. Blood tests: A full blood count assesses red blood cell levels to rule out anaemia. Other targeted tests help identify infections or underlying conditions contributing to low oxygen. Six-minute walk test: This assesses how far you can walk in six minutes and is used to evaluate the functional impact of heart or lung conditions on oxygen delivery during exertion. Treatment for Hypoxia Treatment focuses on restoring adequate oxygen levels and addressing the underlying cause. The specific approach depends on what is causing the hypoxia and how severe it is. Supplemental oxygen: Delivered via nasal prongs, a face mask, or a high-flow oxygen system, this is the first-line treatment for most forms of hypoxia. Inhaled or oral steroids: Used to reduce inflammation and open airways in conditions such as asthma or COPD. Antibiotics: Prescribed when a bacterial infection such as pneumonia is the underlying cause. Blood thinners (anticoagulants): Used to treat pulmonary embolism or blood vessel disease causing circulatory hypoxia. Diuretics: Help remove excess fluid from the lungs in cases of pulmonary oedema or heart failure. Continuous positive airway pressure (CPAP): A mask-based device that keeps the airways open during sleep, used for sleep apnoea. Bilevel positive airway pressure (BiPAP): A more advanced pressure support system used for COPD and certain types of respiratory failure. Mechanical ventilation: In severe or acute cases where breathing is severely compromised, a ventilator in a hospital setting takes over the work of breathing. The prognosis for hypoxia depends on its severity, how quickly it is treated, and the nature of the underlying condition. Many people recover fully when the cause is identified and managed promptly. Others with chronic conditions may require ongoing supplemental oxygen as part of their long-term management. Can Hypoxia Cause Brain Damage? Yes, it can, and the brain is among the most oxygen-sensitive organs in the body. When the brain does not receive enough oxygen, a condition called cerebral hypoxia occurs. Brain cells can begin to die within minutes of severe oxygen deprivation. The extent of damage depends on how severe the hypoxia was and how long it lasted. Mild, brief episodes may cause temporary symptoms such as confusion, headache, or memory lapses. Prolonged or severe cerebral hypoxia can result in lasting cognitive impairment, difficulty with movement, personality changes, or, in the worst cases, permanent brain damage or death. This is why immediate medical attention is essential whenever hypoxia is suspected. Time is critical when the brain is involved. Complications of Untreated Hypoxia When hypoxia goes unrecognised or is not treated in time, it can lead to serious and potentially irreversible consequences: Brain damage, ranging from memory and concentration problems to severe neurological impairment. Heart damage, including heart attack if oxygen supply to the cardiac muscle is severely compromised. Kidney failure, as the kidneys require a constant supply of oxygen-rich blood to filter waste. Respiratory failure, where the lungs are no longer able to maintain adequate gas exchange. Multi-organ failure in severe and prolonged cases. Coma or death in the most extreme circumstances. These outcomes highlight the importance of taking symptoms seriously and seeking prompt care rather than hoping they will resolve on their own. How to Prevent Hypoxia While not all cases of hypoxia are preventable, you can significantly reduce your risk with the following measures: Manage any existing heart or lung condition carefully, including taking prescribed medications consistently and attending regular check-ups. Do not ignore new or worsening respiratory symptoms. Seek medical advice early. Quit smoking. Tobacco use damages the lungs and blood vessels, increasing the risk of conditions that cause hypoxia. If you have asthma, know your triggers, carry your rescue inhaler, and follow your treatment plan. Be cautious about high-altitude travel if you have a heart or lung condition. Speak to your doctor before you travel. Ensure sleep apnoea is properly diagnosed and treated, as it causes repeated overnight dips in oxygen that can have cumulative health effects. Stay physically active and maintain a healthy weight to support cardiovascular and respiratory health. Be aware of the early signs of hypoxia so you can act quickly if they appear. When to Seek Emergency Care Some situations require immediate emergency attention. Do not wait and monitor at home if you or someone around you experiences: Sudden or severe shortness of breath. Bluish or greyish discolouration of the lips, skin, or fingernails. Sudden confusion, extreme restlessness, or a change in consciousness. A rapid heart rate that does not settle. Loss of consciousness or near fainting. Symptoms of a known heart or lung condition that are significantly worse than usual. Any situation where you instinctively feel that something is seriously wrong. Call emergency services immediately in these situations. Hypoxia is a medical emergency and requires prompt, professional intervention. Conclusion Oxygen is fundamental to life, and hypoxia is what happens when that fundamental need goes unmet. Whether caused by a lung condition, a circulatory problem, anaemia, or another underlying issue, hypoxia demands attention and timely medical care. Knowing the signs and understanding the risks puts you in the best position to act quickly when it matters most. Good respiratory and cardiovascular health form the foundation for preventing many causes of hypoxia. Staying proactive about your health, managing chronic conditions, and monitoring key health markers regularly are all meaningful steps you can take. At Metropolis Healthcare, you can access a comprehensive range of health tests, including blood count panels, cardiac markers, and respiratory health investigations, all with the convenience of home sample collection. With over 4,000 tests, fast and accurate reports, and easy booking through the website, app, call, or WhatsApp, staying informed about your health has never been more accessible. Your body gives you signals. Make sure you are listening. Frequently Asked Questions What Are the First Signs of Hypoxia? The earliest signs of hypoxia are often subtle and can be easy to dismiss. Restlessness, headache, mild confusion, and a feeling that you cannot quite get enough air are common early indicators. You may also notice your heart rate increasing or your breathing becoming faster than usual. If any of these symptoms appear without an obvious explanation, it is worth seeking medical assessment promptly rather than waiting to see if they improve. What Oxygen Level Is Considered Low? A normal blood oxygen saturation level, as measured by pulse oximetry, is typically between 95% and 100%. A reading between 91% and 94% is considered mildly low and warrants attention. Anything below 90% is considered significantly low and may indicate hypoxia requiring urgent evaluation. In people with chronic lung conditions, doctors may establish individual target ranges, so always follow your doctor's specific guidance. Can Hypoxia Be Reversed? Yes, in many cases hypoxia can be reversed, particularly when it is identified and treated quickly. Supplemental oxygen, treatment of the underlying cause, and supportive care can restore oxygen levels and allow tissues to recover. The key factor is how long the tissues were deprived of oxygen and how severe the deprivation was. Brief, mild episodes are more likely to resolve completely, while prolonged or severe hypoxia may result in lasting damage, particularly to the brain and heart. Is Hypoxia Life-Threatening? Yes, hypoxia can be life-threatening. Without sufficient oxygen, vital organs including the brain and heart can sustain serious damage within minutes. Severe hypoxia is a medical emergency. Even chronic, lower-grade hypoxia, if left unmanaged, can lead to progressive organ damage over time. This is why it is essential not to underestimate symptoms and to seek medical care without delay when hypoxia is suspected. How Is Hypoxia Treated at Home? Hypoxia itself should not be managed at home without medical guidance, as it is a condition that requires proper diagnosis and treatment. However, people with chronic conditions such as COPD or sleep apnoea may be prescribed home supplemental oxygen or devices like CPAP as part of their long-term management. If you have been given equipment for home use, use it exactly as prescribed. If you develop new or worsening symptoms at any time, do not rely on home devices alone. Contact your doctor or go to the nearest emergency department immediately. References Bhutta BS, Alghoula F, Berim I. Hypoxia. StatPearls. National Library of Medicine; 2023. Martin DS, Grocott MPW. Oxygen therapy in anaesthesia: the yin and yang of O2. Br J Anaesth. 2013;111(6):867-871. Semenza GL. Oxygen sensing, homeostasis, and disease. N Engl J Med. 2011;365(6):537-547. West JB. High-altitude medicine. Am J Respir Crit Care Med. 2012;186(12):1229-1237. Prabhakar NR, Semenza GL. Adaptive and maladaptive cardiorespiratory responses to continuous and intermittent hypoxia mediated by hypoxia-inducible factors 1 and 2. Physiol Rev. 2012;92(3):967-1003. Bateman NT, Leach RM. ABC of oxygen: acute oxygen therapy. BMJ. 1998;317(7161):798-801. Sarkar M, Niranjan N, Banyal PK. Mechanisms of hypoxemia. Lung India. 2017;34(1):47-60.
Blepharospasm: Why Your Eyelids Twitch or Close Involuntarily
Have you ever noticed your eyelid twitching for no clear reason? An occasional flicker is usually harmless and short-lived. But when the twitching becomes frequent, forceful, or difficult to control, it may point to a condition called blepharospasm. Blepharospasm can feel unsettling, especially when it starts interfering with daily tasks like reading, driving, or simply keeping your eyes open. Understanding what it is, why it happens, and how it is treated can help you feel more confident about seeking the right care. What Is Blepharospasm? Blepharospasm is a neurological movement disorder in which the muscles around your eyelids contract involuntarily, causing uncontrollable blinking or eye closure. In mild cases, it may feel like persistent involuntary blinking. In more severe cases, the spasms can force both eyes shut long enough to temporarily affect your vision, even though the eyes themselves are completely healthy. This condition is classified as a type of dystonia, a group of movement disorders caused by abnormal muscle contractions. It primarily involves the orbicularis oculi, the ring-shaped muscle that surrounds each eye and controls eyelid movement. Blepharospasm is relatively rare. Estimates suggest it affects between 128,000 and 2.4 million people worldwide, though the actual number may be higher since many cases go undiagnosed or are attributed to other conditions. Is Blepharospasm the Same as Eye Twitching? It is easy to confuse blepharospasm with common eye twitching, but the two are quite different. Everyday eye twitching, known as myokymia, is usually brief, affects one eye, and resolves on its own after a few minutes or days. It is often triggered by tiredness, caffeine, or eye strain and is generally harmless. Blepharospasm, on the other hand, affects both eyes simultaneously, is involuntary, follows a pattern, and tends to worsen over time without treatment. It is a neurological eye disorder, not a simple muscle twitch. If your eyelid twitching is frequent, bilateral, forceful, or disrupting your daily life, it warrants medical attention. Types of Blepharospasm Blepharospasm is broadly divided into two types: Primary blepharospasm: Also called benign essential blepharospasm (BEB), this form occurs on its own without a clearly identifiable cause. It is classified as idiopathic, meaning the exact origin is not yet fully understood. Despite the word benig in its name, it can still significantly impact quality of life. Secondary blepharospasm: This form develops as a result of another underlying condition. It is essentially a symptom of something else happening in the body, such as an inflammatory eye condition, a movement disorder, or a medication side effect. Treating the root cause often helps reduce or resolve the spasms. Common Causes of Blepharospasm The exact cause of blepharospasm is not always clear, particularly for the primary form. However, research points to the following potential causes: Neurological dysfunction: Irregular activity in the basal ganglia, the part of the brain that coordinates movement, is thought to play a key role. Abnormal signalling through the facial nerve (Cranial Nerve VII), which controls eyelid muscles, may also contribute. Underlying eye conditions: Conditions such as dry eyes, blepharitis (eyelid inflammation), and keratoconjunctivitis (eye surface inflammation) can trigger reflex blepharospasm. These conditions often cause eye strain or a burning sensation before spasms develop. Other movement disorders: Meige syndrome, a condition that involves spasms in the face and jaw alongside the eyes, is a known cause. Atypical forms of parkinsonism have also been linked to blepharospasm. Medications: Certain drugs, particularly those used in the treatment of Parkinson's disease, can cause involuntary muscle movements as a side effect. A condition called tardive dyskinesia, linked to long-term use of some medications, can also increase risk. Lifestyle and environmental triggers: Stress, sleep deprivation, excessive caffeine intake, alcohol consumption, smoking, and exposure to bright light can all trigger or worsen blepharospasm episodes. Genetic factors: Around 20 to 30 percent of people with blepharospasm have a family member with the same condition, suggesting a hereditary component. Symptoms of Blepharospasm Blepharospasm starts subtly and tends to progress over time. Recognising the symptoms early can help you seek timely care. Frequent, uncontrollable blinking that cannot be consciously stopped Involuntary blinking that is more pronounced than usual, even between active spasm episodes Spasms affecting both eyes simultaneously Spasms that follow a pattern rather than occurring randomly Forced eye closure lasting a few seconds to several minutes Temporary visual impairment during severe spasms, not due to any damage to the eye Sensitivity to bright light (photophobia) Eye irritation, dryness, or a burning sensation, particularly in secondary blepharospasm Brief improvement of spasms with sensory tricks such as humming, touching the face, or concentrating on a task Symptoms typically begin with mild, occasional twitching and gradually become more frequent and forceful. In severe cases, the spasms can make it difficult to drive, work, or read. Risk Factors for Blepharospasm Certain factors increase the likelihood of developing blepharospasm: Sex: Women are two to four times more likely to develop blepharospasm than men, and their symptoms may also be more severe. Age: The condition most commonly develops between the ages of 50 and 70. Family history: Having a biological relative with blepharospasm raises your risk. Chronic stress: High stress levels can trigger episodes and increase their frequency. Fatigue: Insufficient sleep or physical exhaustion can worsen spasms. Eye health history: Previous eye injuries, chronic eye conditions, or a history of nervous system conditions increase vulnerability. Mental health conditions: Conditions such as anxiety, depression, and obsessive-compulsive disorder (OCD) have been associated with blepharospasm, though the exact relationship between them is still being studied. How Blepharospasm Is Diagnosed Diagnosing blepharospasm can take time, and it often requires input from more than one specialist. Here is what you can typically expect: Medical history review: Your doctor will ask about when the symptoms started, how often they occur, what seems to trigger or relieve them, and whether any family members have had similar issues. Physical and neurological examination: A thorough examination helps assess the nature of the spasms, how they affect your eyelids, and whether there are any other neurological signs. Ophthalmological assessment: An eye specialist may examine your eyes for surface conditions, inflammation, or dryness that could be contributing to the spasms. Electromyography (EMG): This test measures the electrical activity in muscles and can help confirm abnormal muscle contractions around the eyes. MRI or additional imaging: These may be ordered to rule out other neurological conditions that could be causing similar symptoms. Because blepharospasm shares features with several other conditions, it is common for people to see both an ophthalmologist and a neurologist before a definitive diagnosis is reached. Treatment Options for Blepharospasm There is currently no permanent cure for blepharospasm, but several effective treatments can manage symptoms and significantly improve quality of life. Botulinum toxin injections: This is the most common and effective first-line treatment. Small amounts of botulinum toxin are injected into the muscles around the eyes to temporarily reduce their ability to contract. The effects typically last three to four months, after which repeat injections are needed. Most people tolerate the procedure well and experience meaningful relief. FL-41 tinted lenses: These specialised lenses filter out certain wavelengths of light, particularly blue light, which helps reduce photosensitivity and lessen spasm frequency. They are widely available and can be made with prescription lenses if needed. Oral medications: In some cases, doctors may prescribe medications to help manage spasms, though these are generally considered less effective than injections. Surgery (myectomy): For severe cases that do not respond adequately to injections, surgery to partially remove or thin the overactive eyelid muscles may be recommended. It is considered a last resort but can provide lasting relief for those who need it. Acupuncture: Some research suggests acupuncture may offer benefit for certain individuals, and your doctor may consider it as a complementary option. Lifestyle adjustments: Managing stress, getting adequate sleep, reducing caffeine and alcohol intake, and wearing sunglasses in bright conditions can all help reduce the frequency and severity of episodes. Treating underlying causes: If blepharospasm is secondary to another condition such as dry eyes or blepharitis, treating that condition directly often reduces spasms. Complications of Untreated Blepharospasm While blepharospasm is not life-threatening, leaving it untreated can have a significant impact on daily life. Progressive worsening of spasms, eventually making it difficult or impossible to keep the eyes open Inability to drive safely, which can limit independence Difficulty with tasks that require sustained visual attention, such as reading, working on a screen, or watching television Increased risk of falls or injuries during episodes of forced eye closure Social withdrawal due to embarrassment or the fear of having a spasm in public Emotional consequences, including heightened anxiety, depression, and social isolation Seeking treatment early helps minimise these complications and preserve a good quality of life. Can Blepharospasm Be Prevented? Unfortunately, blepharospasm cannot be fully prevented, and there is no known way to eliminate your risk of developing it. However, some measures may help reduce the frequency or severity of episodes: Managing stress through relaxation techniques, mindfulness, or physical activity Prioritising regular, restful sleep Wearing tinted or protective eyewear in bright environments Reducing consumption of caffeine and alcohol Addressing underlying eye conditions like dryness or inflammation promptly Identifying and using sensory tricks that personally work for you If you have a family history of blepharospasm, being aware of early symptoms can help you seek medical attention sooner. When to See a Doctor It is worth speaking to a doctor if: Your eyelid twitching has persisted for more than a few weeks The twitching affects both eyes The spasms are forceful enough to close your eyes Your vision is affected during episodes The twitching is interfering with driving, work, or daily activities You notice increased sensitivity to light alongside the twitching The symptoms are causing anxiety or affecting your emotional wellbeing Early evaluation helps confirm the diagnosis, rule out other causes, and start treatment before symptoms progress further. Frequently Asked Questions What Causes Eyelid Twitching? Occasional eyelid twitching is usually caused by tiredness, stress, eye strain, or too much caffeine. These twitches are harmless and typically resolve on their own. When twitching is frequent, affects both eyes, and cannot be controlled, it may indicate blepharospasm, a neurological eye disorder involving abnormal activity in the brain's movement control system or the facial nerve. Can Blepharospasm Be Prevented? Blepharospasm cannot be prevented entirely. However, managing known triggers such as stress, fatigue, bright light, and excessive caffeine may help reduce how often and how severely symptoms occur. Regular eye care and prompt treatment of conditions like dry eyes can also be helpful, particularly for the secondary form. Is Blepharospasm Serious? Blepharospasm is not life-threatening, but it can be seriously disruptive. In severe cases, it can temporarily impair vision and limit your ability to drive, work, or carry out everyday tasks. It can also affect mental wellbeing, leading to anxiety and social avoidance if left unmanaged. With appropriate treatment, most people can achieve significant symptom relief and maintain a good quality of life. Can Stress Cause Blepharospasm? Stress is a well-recognised trigger for blepharospasm. It does not necessarily cause the condition, but it can initiate episodes and increase their frequency or severity. Managing stress through regular exercise, adequate sleep, and relaxation practices can help reduce the impact of blepharospasm on daily life. Does Blepharospasm Go Away? In most cases, primary blepharospasm is a long-term condition. Research suggests that it resolves spontaneously in approximately 11 percent of cases, though more evidence is needed to understand when and why this happens. Secondary blepharospasm may improve or resolve when the underlying cause is treated effectively. What Is the Best Treatment for Blepharospasm? Botulinum toxin injections are currently the most effective treatment for blepharospasm. They offer significant relief from spasms for most people and are typically repeated every three to four months. For those who do not respond well to injections, surgical options are available. Lifestyle modifications and tinted lenses can also be useful as complementary measures. Take Charge of Your Eye Health with Metropolis Healthcare If you are noticing persistent or worsening eyelid spasms, understanding your overall health picture is an important first step. While blepharospasm is primarily a neurological condition, certain underlying factors such as vitamin D levels, inflammatory markers, and general health can play a role in how your body functions. Metropolis Healthcare offers a comprehensive range of diagnostic tests to help you and your doctor build a clearer picture of your health. From routine blood panels to speciality tests, Metropolis brings accurate, reliable results with the convenience of home sample collection, quick turnaround times, and easy booking through the website, app, call, or WhatsApp. Taking a proactive approach to health monitoring is always a good idea, whether you are managing a specific condition or simply staying ahead of potential concerns. Book your tests with Metropolis Healthcare today and take one confident step towards better health. References Defazio G, Hallett M, Jinnah HA, Berardelli A. Development and validation of a clinical guideline for diagnosing blepharospasm. Neurology. 2013;81(3):236-240. Jankovic J, Kenney C, Grafe S, Goertelmeyer R, Comes G. Relationship between various clinical outcome assessments in patients with blepharospasm. Mov Disord. 2009;24(3):407-413. Evidente VG, Adler CH. An update on the neurological applications of botulinum toxins. Curr Neurol Neurosci Rep. 2010;10(5):338-344. Roggenkamper P, Jost WH, Bihari K, et al. Efficacy and safety of a new botulinum toxin type A free of complexing proteins in the treatment of blepharospasm. J Neural Transm. 2006;113(3):303-312. Vagefi MR, Lin CC, McCann JD, Anderson RL. Myectomy for blepharospasm. Ophthalmic Plast Reconstr Surg. 2009;25(5):374-377. Hallett M, Evinger C, Jankovic J, Stacy M. Update on blepharospasm: report from the BEBRF International Workshop. Neurology. 2008;71(16):1275-1282. Grandas F, Elston J, Quinn N, Marsden CD. Blepharospasm: a review of 264 patients. J Neurol Neurosurg Psychiatry. 1988;51(6):767-772.
Varicella Zoster Virus and the Diseases It Causes
Most people associate chickenpox with a childhood memory of an itchy rash, a week at home, and perhaps some calamine lotion. What many do not realise is that the virus responsible for that childhood illness never truly leaves the body. It retreats into the nervous system and can resurface decades later as a far more painful condition called shingles. Understanding the varicella zoster virus, how it behaves, and what it can do helps you protect yourself and your family at every stage of life. What Is Varicella Zoster Virus? Varicella zoster virus (VZV) is a member of the herpes virus family. It is the single virus responsible for two distinct diseases. The first time you encounter VZV, it causes chickenpox (varicella), a highly contagious illness characterised by an itchy, blister-like rash. After the illness resolves, the virus does not leave the body. Instead, it travels into the sensory nerve roots of the spinal cord, where it remains dormant, sometimes for decades. In some people, years or even decades later, the virus reactivates. This second episode is called shingles, or herpes zoster. It typically causes a painful, localised rash along a specific band of skin supplied by the affected nerve. Beyond chickenpox and shingles, VZV reactivation can occasionally affect the eyes, the facial nerves, and in rare cases, the brain and its surrounding membranes. How Varicella Zoster Virus Spreads VZV is one of the most contagious viruses known. Understanding how it spreads is key to limiting its transmission. Respiratory droplets: During a chickenpox infection, the virus spreads through the air when an infected person coughs or sneezes. You can inhale the virus even without direct contact. Direct contact with the rash: Touching the fluid from a chickenpox rash or a shingles rash can transmit the virus to someone who has not been previously infected or vaccinated. Airborne particles from blisters: During reactivation (shingles), tiny particles from the rash can sometimes carry the virus through the air in close proximity. From shingles to unvaccinated individuals: You cannot catch shingles from someone who has it. However, an unvaccinated person who has never had chickenpox can contract chickenpox through contact with an active shingles rash. A person with chickenpox is contagious from about one to two days before the rash appears until all blisters have completely crusted over. During this window, isolation is essential to prevent spread, particularly to vulnerable individuals. Causes of Varicella Zoster Infection VZV infection occurs in two stages, each with a distinct trigger: Primary infection (chickenpox): Caused by first exposure to the virus, most commonly in childhood. The virus enters through the respiratory tract and spreads throughout the body, causing the characteristic chickenpox rash. Reactivation (shingles): After the primary infection, the virus lies dormant in the dorsal root ganglia of the spine or in the trigeminal nerve of the face. When the immune system is weakened or under stress, the virus can reactivate and travel along the nerve pathway to the skin, producing the shingles rash. No prior chickenpox needed for exposure: People who were vaccinated but never had natural chickenpox can still develop a milder form of the illness if exposed to the virus, though their symptoms are typically less severe. Risk Factors for Severe Infection While most healthy children recover from chickenpox without complications, certain groups are at higher risk of a more serious illness: Adults who contract chickenpox for the first time tend to experience more severe symptoms than children. People aged 50 and above are at significantly increased risk of shingles reactivation and its complications. Individuals taking immunosuppressive medications, such as those used after organ transplants or for autoimmune conditions. People living with conditions that weaken the immune system, including HIV, cancer, or those undergoing chemotherapy. Pregnant women, who face particular risks to themselves and their unborn baby. Newborns whose mothers contract chickenpox just before or after delivery. People under significant physical or emotional stress, which can temporarily suppress immune function. Symptoms of Varicella Zoster Virus Infection Symptoms differ depending on whether VZV is causing a primary infection or a reactivation. Chickenpox symptoms: A widespread, intensely itchy chickenpox rash that begins as small red spots, progresses to fluid-filled blisters, and then crusts over. The rash typically starts on the face, chest, and back before spreading to the rest of the body. Fever, often mild to moderate. Fatigue and a general feeling of being unwell. Headache. Loss of appetite. The chickenpox rash usually lasts seven to ten days from first appearance to complete crusting. Shingles symptoms: Pain, burning, or tingling along a band of skin, often preceding the rash by several days. A localised shingles rash that appears as a stripe of blisters, typically on one side of the body or face, following the path of a single nerve. Sensitivity of the affected skin even to light touch. Fever and headache in some cases. In cases involving the eye area (herpes zoster ophthalmicus): eye redness, swelling, and sensitivity to light. In cases involving the facial nerve (Ramsay Hunt syndrome): ear pain, facial paralysis, and sometimes hearing changes. Complications of Varicella Zoster Most cases of chickenpox resolve without lasting effects. However, complications can occur, particularly in high-risk groups: Bacterial skin infections from scratching open blisters. Pneumonia, which can be serious in adults and immunocompromised individuals. Encephalitis, a rare but dangerous inflammation of the brain. Meningitis or meningoencephalitis, affecting the brain and its surrounding membranes. Dehydration, particularly in young children or those who develop sores in the mouth. Reye's syndrome in children given aspirin during a chickenpox illness (aspirin should be avoided in children with viral infections). Shingles carries its own set of complications: Postherpetic neuralgia (PHN): Persistent nerve pain in the affected area that continues long after the rash has healed. This is the most common complication of shingles and can last for months or years. Vision loss: When shingles affects the eye (herpes zoster ophthalmicus), it can damage the cornea and threaten sight if not treated promptly. Hearing loss or facial paralysis: In Ramsay Hunt syndrome, VZV reactivation in the facial nerve can cause these serious effects. Bacterial superinfection of the shingles rash. Varicella Zoster in Children Chickenpox is primarily a childhood illness and is generally milder in children than in adults. Most children develop a moderate number of blisters, a low-grade fever, and some discomfort over the course of one to two weeks. Healthy children typically recover fully without complications. That said, certain children are at higher risk of complications. Newborns, very young infants, and children with weakened immune systems can develop severe chickenpox that requires hospitalisation and antiviral treatment. Children who have been vaccinated against chickenpox are either protected from infection or experience a significantly milder form if they do contract the virus. Learning to recognise chickenpox symptoms early helps parents seek appropriate care promptly and take steps to prevent spreading the illness to others. Varicella Zoster in Adults Chickenpox is less common in adults because most were exposed during childhood, but when it does occur in adults who missed the infection or vaccination, it tends to be considerably more severe. Adults with chickenpox are at greater risk of pneumonia, hospitalisation, and other complications compared to children. Shingles, on the other hand, is predominantly an adult condition. Around one in three people will develop shingles at some point in their lifetime. The risk rises sharply after the age of 50 and continues to increase with age. Older adults are also more likely to develop postherpetic neuralgia, the persistent nerve pain that can follow a shingles episode and significantly impair quality of life. Varicella Zoster in Pregnancy Chickenpox during pregnancy poses risks to both the mother and the developing baby. Pregnant women are more likely to develop severe chickenpox with complications including pneumonia, which can be life-threatening. The timing of infection during pregnancy also matters greatly for the baby. Chickenpox contracted in the first 20 weeks of pregnancy carries a small but real risk of foetal varicella syndrome, which can cause skin scarring, limb abnormalities, eye problems, and neurological damage in the baby. If a pregnant woman develops chickenpox within five days of delivery or up to two days after, the newborn is at risk of severe neonatal chickenpox, as the baby has not yet received protective antibodies from the mother. Pregnant women who have not had chickenpox and have not been vaccinated should avoid contact with anyone who has an active infection and seek immediate medical advice if they believe they have been exposed. Vaccination is not given during pregnancy, but women planning to conceive can be vaccinated beforehand. How Varicella Zoster Is Diagnosed In most cases, a doctor can diagnose chickenpox or shingles based on the characteristic appearance and distribution of the rash. However, laboratory confirmation is sometimes needed, particularly in atypical presentations or in immunocompromised patients. Clinical assessment: The doctor evaluates the appearance, location, and progression of the rash alongside the patient's symptoms and history of previous chickenpox or vaccination. Polymerase chain reaction (PCR) test: A highly sensitive test performed on fluid taken from the blisters or a swab of the rash. It detects the genetic material of VZV and is considered the most accurate diagnostic method. Direct fluorescent antibody (DFA) test: A rapid test using blister fluid or tissue to identify VZV antigens under a fluorescent microscope. Viral culture: A sample from the rash is used to grow the virus in a laboratory. This method takes longer than PCR but can confirm active infection. Blood tests for antibodies: VZV-specific IgM and IgG antibody tests can indicate whether someone is experiencing a current infection, has had a previous infection, or has developed immunity through vaccination. Imaging: In cases where neurological complications such as encephalitis or meningitis are suspected, brain imaging and a lumbar puncture may be needed. Treatment for Varicella Zoster There is no cure for VZV. Once in the body, the virus remains there for life. However, antiviral medications can reduce the severity and duration of both chickenpox and shingles, and are particularly important in high-risk individuals. Antiviral medications: Acyclovir, valacyclovir, and famciclovir are the main antivirals used. They work most effectively when started early, ideally within 72 hours of the rash appearing. Pain relief: Over-the-counter or prescription pain medications help manage the discomfort of both chickenpox and shingles. Soothing measures for chickenpox: Calamine lotion, cool baths, and antihistamines can help relieve itching. Keeping fingernails short and clean helps prevent secondary infection from scratching. Wound care: Keeping blisters clean and avoiding bursting them reduces the risk of bacterial skin infection. Corticosteroids: Occasionally used in combination with antivirals for severe shingles to reduce inflammation, though this is determined on a case-by-case basis. Postherpetic neuralgia management: Nerve pain following shingles may be treated with specific medications including certain antidepressants, anticonvulsants, or topical patches and creams, under medical supervision. Varicella Zoster Vaccination Vaccination is the most effective way to prevent both chickenpox and shingles. The chickenpox vaccine is given as part of routine childhood immunisation schedules and is highly effective at preventing infection or significantly reducing its severity. Adults who have never had chickenpox or been vaccinated can receive the vaccine. A shingles vaccine is recommended for adults aged 50 and above, regardless of whether they remember having had chickenpox. Even those who have already had shingles can benefit from vaccination to reduce the risk of recurrence. Vaccination not only protects the individual but also reduces the risk of transmission to vulnerable people who cannot be vaccinated, such as newborns and immunocompromised individuals. The vaccines are safe, well-studied, and are not given to pregnant women or people with severely compromised immune systems. Speak to your doctor about the most appropriate timing and type of vaccine for your circumstances. When to See a Doctor In many cases, chickenpox in healthy children can be managed at home with supportive care. However, seek medical advice if: You are an adult who has developed chickenpox for the first time. You are pregnant and have been exposed to or developed chickenpox. Your child has an underlying condition that weakens the immune system. The rash appears to be infected, with increasing redness, warmth, or pus. Symptoms of shingles appear, particularly in adults over 50 or those who are immunocompromised. The shingles rash involves the eye area or the face. Seek emergency care immediately if you or anyone in your care develops: Confusion or altered mental state. A severe or persistent headache. A stiff neck. Sores on the eyes or sudden vision changes. Difficulty breathing. A very high fever that does not settle. Extreme difficulty waking up. Conclusion Varicella zoster virus is a lifelong companion that most people acquire in childhood, often without understanding the full picture of what it can mean later in life. Chickenpox is usually manageable, but shingles can cause considerable suffering, and in vulnerable individuals, both conditions can become serious. Vaccination remains the most powerful tool available for prevention, both in childhood and in later adulthood. Staying proactive about your health is the best way to stay a step ahead. At Metropolis Healthcare, a comprehensive range of tests is available to support your wellbeing at every life stage, from immunity-related assessments to full body health checks. With home sample collection across a wide network of touchpoints, over 4,000 tests, accurate reports, and easy booking through the website, app, call, or WhatsApp, taking charge of your health has never been simpler. Prevention starts with awareness. Make it count. Frequently Asked Questions Is Varicella Zoster Contagious? Yes, varicella zoster virus is highly contagious. Chickenpox spreads through respiratory droplets and direct contact with the rash. A person with chickenpox is contagious from one to two days before the rash appears until all blisters have crusted over. Shingles itself cannot be passed from one person to another as shingles. However, someone who has never had chickenpox and is not vaccinated can contract chickenpox from direct contact with a shingles rash. Can Varicella Zoster Be Prevented? Yes. The most effective prevention is vaccination. The chickenpox vaccine is given as part of routine childhood immunisation and is highly protective. A shingles vaccine is recommended for adults aged 50 and over. Good hygiene practices, avoiding contact with infected individuals, and covering an active rash are also important measures to limit spread. Can You Get Shingles Without Having Had Chickenpox? Not through natural infection. Shingles is a reactivation of VZV that has already been present in your body since a prior chickenpox infection. If you have never had chickenpox or been vaccinated, you cannot develop shingles from VZV. However, in very rare cases, those who received the chickenpox vaccine may occasionally develop a mild form of shingles, as the vaccine contains a weakened form of the live virus. How Long Does Chickenpox Last? The chickenpox rash typically progresses over seven to ten days. It begins as small red spots, develops into fluid-filled blisters, and gradually dries out and crusts over. The entire illness, including fever and other symptoms, usually resolves within ten to fourteen days in otherwise healthy children. Adults and immunocompromised individuals may experience a more prolonged and severe illness. Is Shingles Dangerous? Shingles can be painful and debilitating, and it does carry the risk of serious complications. The most common is postherpetic neuralgia, which is persistent nerve pain that can last for months or years after the rash heals. Shingles affecting the eye can threaten vision, and in rare cases, the virus can affect the brain. People over 60 and those with weakened immune systems are at the greatest risk of severe disease and complications. Early antiviral treatment significantly reduces the severity and the risk of complications. Does Vaccination Prevent Shingles? Yes. The shingles vaccine significantly reduces the risk of developing shingles and, in those who do get it despite vaccination, greatly reduces the severity of the illness and the risk of postherpetic neuralgia. It is recommended for adults aged 50 and above, including those who have already had shingles. The vaccine does not guarantee complete protection but offers a meaningful and well-established reduction in risk. References Arvin AM. Varicella-zoster virus. Clin Microbiol Rev. 1996;9(3):361-381. Gershon AA, Breuer J, Cohen JI, et al. Varicella zoster virus infection. Nat Rev Dis Primers. 2015;1:15016. World Health Organization. Varicella and herpes zoster vaccines: WHO position paper. Wkly Epidemiol Rec. 2014;89(25):265-288. Johnson RW, Alvarez-Pasquin MJ, Bijl M, et al. Herpes zoster epidemiology, management, and disease and economic burden in Europe: a multidisciplinary perspective. Ther Adv Vaccines. 2015;3(4):109-120. Oxman MN, Levin MJ, Johnson GR, et al. A vaccine to prevent herpes zoster and postherpetic neuralgia in older adults. N Engl J Med. 2005;352(22):2271-2284. Gnann JW Jr, Whitley RJ. Herpes zoster. N Engl J Med. 2002;347(5):340-346. Centers for Disease Control and Prevention. Chickenpox (Varicella): For healthcare professionals. CDC; 2023.