Preventive Healthcare
Bedsores (Pressure Ulcers): Causes, Stages, Treatment, and Prevention Strategies
1161 Views
0
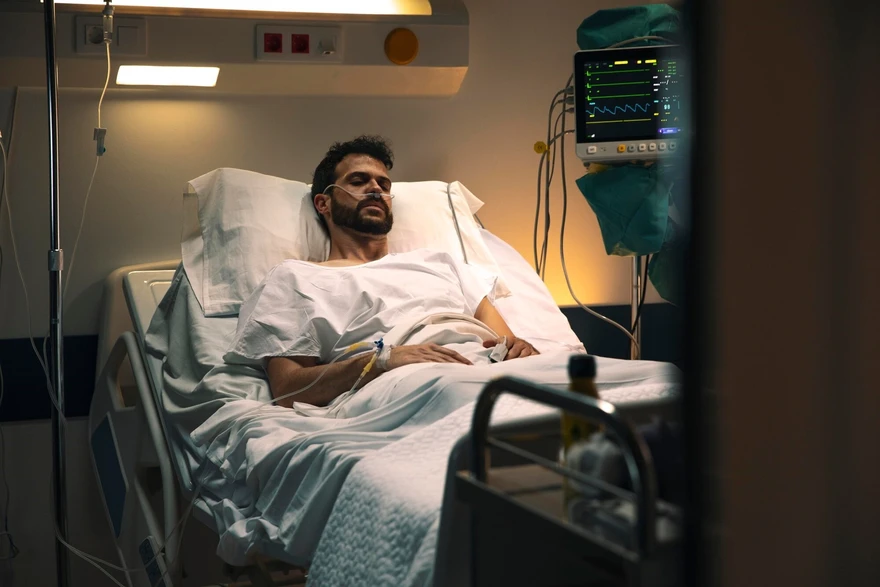
What are bedsores?
Bedsores are injuries to the skin and underlying tissues resulting from prolonged pressure on the skin. They can be an unfortunate and common occurrence among people who are bedridden or generally immobile, such as those in wheelchairs. Bedsores usually develops on the skin which is covering the bony areas of the body such as the heels, ankles, hips, tailbone, and shoulder blades.
What are other names for bedsores?
Bedsores are also known as pressure sores or pressure ulcers.
How common are bedsores?
Bedsores are relatively common among immobile or bedridden people, especially in hospitals and nursing homes. They are a serious health problem for patients in all kinds of settings, from large hospitals to long-term care facilities and residential care facilities. Bedsores are associated with lengthy and costly hospital stays.
What parts of your body do Bedsores affect?
Bedsores usually occur on the back, buttocks, hips, heels, elbows, and other areas that bear weight or are subject to pressure during immobility. These areas are more prone to bedsores due to reduced blood flow and prolonged pressure, which can lead to tissue damage. Correct body positioning, regular movement and good skin care are key to preventing bedsores in vulnerable people.
What causes Bedsores?
Bedsores causes primarily occur due to prolonged pressure on the skin which leads to a decreased blood supply to the area. This lack of oxygen and nutrients can cause skin cells to die, leading to bedsores.
Some factors that contribute to bedsore causes include:
- Constant Pressure: Pressure applied on your skin and makes the blood circulation difficult to that area. Due to which your skin can’t get enough oxygen or nutrients. This weakens the skin and causes cells to die.
- Friction: Rubbing against clothing or bedding can damage sensitive skin
- Shear: Skin that stretches or pulls due to movement can increase pressure sore risk
Who is at risk for Bedsores?
People who are bedridden, wheelchair-bound, or have limited mobility are more prone to bedsores. Additionally, older adults, individuals with sensory or neurological impairments, and those with compromised circulation are more susceptible to bedsores.
What health conditions increase your risk of Bedsores?
Health conditions such as paralysis, diabetes, vascular disease, and spinal cord injury increase the risk of bedsores. In addition, poor nutrition, dehydration, and prolonged pressure on the skin and tissues further increase the likelihood of developing these pressure ulcers or bedsores.
What are the signs of Bedsores?
Signs may include changes in the colour or texture of the skin, swelling or areas of tenderness. It's important to regularly check for these signs, especially in bony areas of the body. Early detection is crucial in effective bedsores treatment.
What are the stages of Bedsores?
Depending on their severity, bedsores can range from stage I (mild) to stage IV (severe). Understanding these stages of bedsores can help in identifying their progress and hence in determining appropriate bedsores treatment plans:
- Stage I: This is the mild stage. Here, bedsores only affect the top layer of skin due to which the skin appears red and warm, with discomfort or itching
- Stage II: This happens when the wound goes deeper below the surface of your skin. Because of this, the skin tears and may look like a blister or abrasion
- Stage III: These sores have penetrated in the second layer of skin into the fat tissue, and extends into the tissue beneath the skin, forming a small crater.
- Stage IV: These sores are the most serious. Some can be so deep that they affect muscles, ligaments and bones.
In addition to these stages of bedsores, sometimes it may be unstageable or involve any suspected deep tissue injury.
What are the complications of Bedsores?
If left untreated, bedsores can cause some serious complications. These may include skin infections, sepsis, and amputations due to severe infection or even cancer in extremely protracted cases. It also increases the risk of life-threatening bacterial infections, such as cellulitis and sepsis.
What are the signs of an infected Bedsore?
An infected bedsore may present as swelling, warmth around the wound site, foul odour or pus. If a bedsore shows signs of infection, a prompt medical attention is needed.
How are Bedsores diagnosed?
The diagnosis process for bedsores begins with a thorough physical examination. Your doctor may ask you questions like when the sores appear or whether they are painful to determine if you have a bedsore and if so, what stage it's in. If there is any suspicion of an infection, further tests like blood tests, biopsies, or imaging might be conducted.
What are nonsurgical treatments for Bedsores?
Nonsurgical treatments for bedsores focus on relieving pressure, promoting healing, and preventing infection. These bedsores treatments includes regularly changing the body position to relieve pressure on the area, using special cushions or mattresses to distribute weight evenly, and keeping the skin clean and dry.
Dressings and topical treatments like antibiotics or medicated bedsores cream may be used to manage wounds and prevent infections. Additionally, improving nutrition with a balanced diet rich in protein and vitamins supports tissue repair. Physical therapy helps maintain mobility and circulation, crucial for bedsore prevention.
What medications treat Bedsores?
In case of pain from bedsores, nonsteroidal anti-inflammatory drugs could be used for relief. These include medications like ibuprofen or naproxen sodium. Using them before changing positions or cleaning the wounds can help manage the discomfort. In case of infected bedsores, antibiotics might be required.
What are surgical treatments for Bedsores?
In more serious cases of bedsores, particularly in stage IV, immediate medical attention is required, which might lead to surgical intervention. One common surgical treatment for bedsores is skin grafting. Which involves transplanting skin or muscle from another part of your body to cover the sore.
How can you prevent Bedsores?
Bedsores prevention involves proactive measures to reduce pressure on vulnerable areas and maintain skin health.
- Changing your body position regularly and using cushions or specialised mattresses can help reduce pressure points, which is very important in bedsores prevention.
- Keeping your skin clean and moisturised prevents dryness and irritation which can contribute to skin breakdown.
- Encouraging movement and exercises to improve circulation and muscle tone is essential, especially for immobile individuals.
- Monitoring nutrition and hydration levels supports skin integrity and overall health, aiding in bedsores prevention.
- Regular assessments by healthcare providers can help identifying early signs of skin damage, and enabling timely interventions such as dressing changes or adjustments in positioning to prevent bedsores from developing or worsening.
What is the outlook for someone with Bedsores?
Most people can recover from bedsores completely with timely detection and treatment. However, those who are at a risk should be vigilant to prevent serious recurrence.
When to see a doctor?
You should consult your healthcare provider if you notice signs of bedsores – like red or discoloured skin that doesn't lighten when touched – especially if you're housebound or wheelchair-bound.
What’s the role of a nutritious diet when you have Bedsores?
A nutritious diet boosts the overall health and aids in faster healing of bedsores. Include foods rich in proteins, vitamins A and C, and the minerals iron and zinc in your diet.
Conclusion
Understanding bedsores, their causes, and treatment options is pivotal to preventing and managing them effectively. Regular position changes, good skin care, a nutritious diet, and professional medical advice are the crucial elements which aids in managing this health condition.
Metropolis Healthcare offers a reliable range of diagnostic services, including at-home sample collection for various tests. The reports are conveniently shared online via email or the Metropolis TruHealth app. The expertise and patient-centric approach of Metropolis Healthcare empower patients to prioritise their health effectively.






















 WhatsApp
WhatsApp